Home
Locations 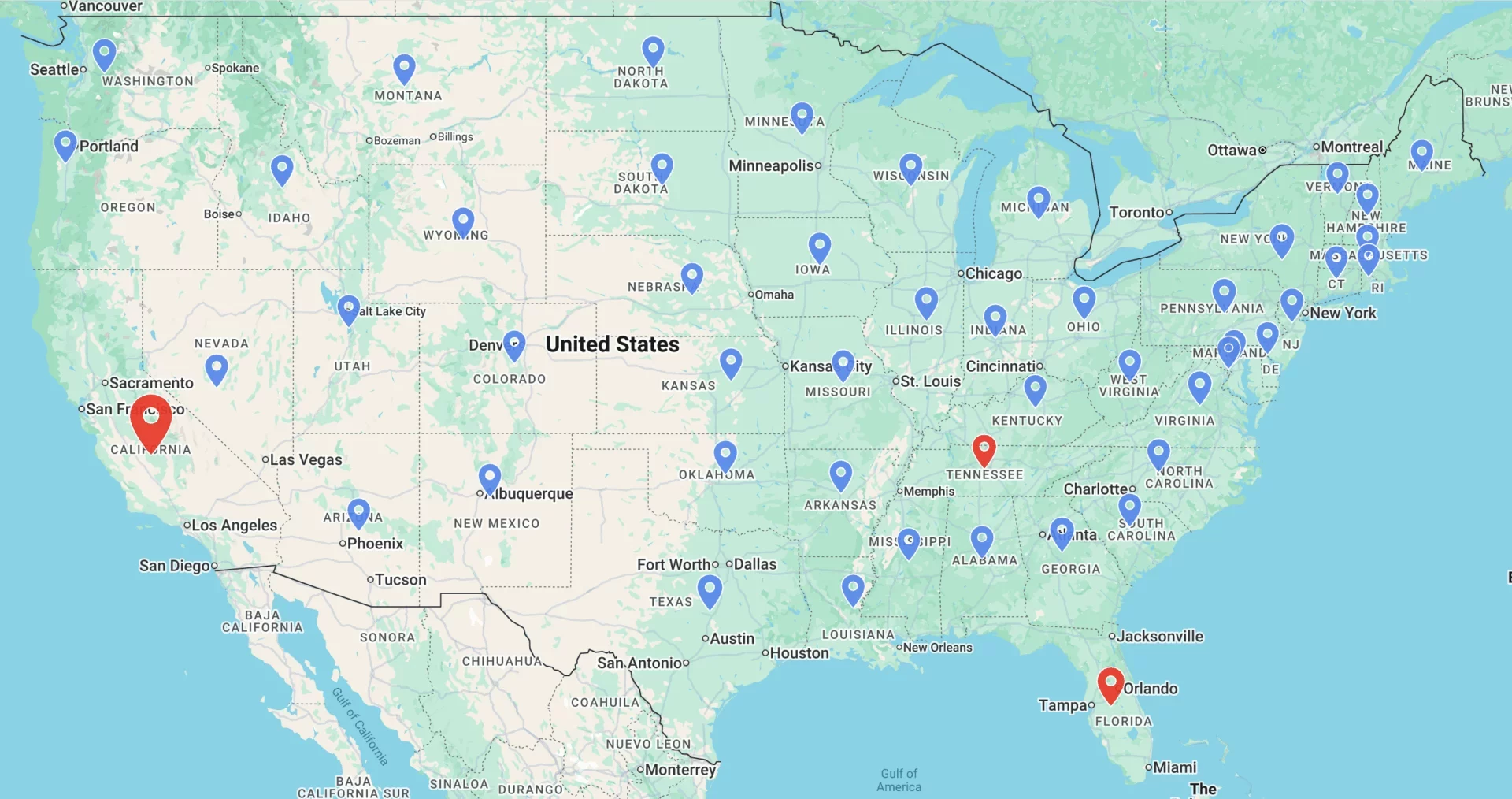
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions

Home
Locations 
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions








Matthew D'Ursov

Amy Leifeste

Karena Mathis



Benzodiazepine use often starts as a prescribed solution for anxiety, sleep issues, or panic, but over time it can quietly reshape daily functioning. Dependence may develop even when medication is taken as directed, leading to memory issues, emotional flattening, increased anxiety, or fear of stopping due to withdrawal symptoms. Many people feel unsure whether they need rehab or how to taper safely, which can delay treatment and prolong discomfort.
• Benzo use can affect memory, mood, and emotional regulation
• Dependence may develop even with prescribed use
• Withdrawal symptoms make stopping feel risky
• Structured rehab supports safe, gradual stabilization
Renaissance Recovery offers Benzo Rehab through the District Behavioral Health network, providing structured outpatient care focused on safety, gradual tapering, and emotional stability. For individuals whose benzodiazepine use is closely connected to anxiety, trauma, or mood disorders rather than addiction alone, benzo-related mental health treatment is also available through Connections Mental Health, part of the DBH family of care. These programs work together to match treatment to individual needs.
Benzo rehab helps restore clarity and stability. See more about our benzo rehab program below.
Our behavioral health services support men and women struggling with substance use and co-occurring mental health disorders. District Behavioral Health focuses on providing a comprehensive continuum of care, including personalized outpatient treatment, intensive outpatient (IOP) and partial hospitalization programs (PHP), and coordinated support services designed to help individuals stabilize, develop effective coping skills, and build lasting recovery within their communities.
Benzodiazepine addiction is a serious condition that can significantly impact a person’s mental and physical health, making it extremely difficult to stop using the medication without professional support. At District Behavioral Health, our specialized treatment centers provide the medical supervision, counseling, and recovery tools necessary to overcome dependence safely and effectively.
This article explains what benzodiazepine addiction is, when treatment becomes necessary, and how professional care can support long-term recovery.
Benzodiazepine addiction occurs when a person develops a physical or psychological dependence on this class of medications, which are commonly prescribed for anxiety, insomnia, and seizures. Often called “benzos,” this category includes well-known drugs like Xanax, Valium, Ativan, and Klonopin. They work by producing a calming effect on the brain and body, but this mechanism also makes them prone to dependence, especially with long-term or high-dose use.
While physicians prescribe these drugs for their effectiveness in providing short-term relief, their calming properties can lead to misuse. A person might start taking higher doses than prescribed or continue using them longer than recommended. Over time, the body builds a tolerance, meaning more of the drug is needed to achieve the same effect. This cycle can quickly escalate into a full-blown addiction [1].
Dependence on benzodiazepines is not just about misuse; it involves the brain and body adapting to the presence of the drug. When someone attempts to stop suddenly, they can experience severe withdrawal symptoms, including intense anxiety, tremors, and, in some cases, life-threatening seizures. This makes quitting without medical support incredibly dangerous and is why professional treatment, starting with a structured detox, is essential for a safe recovery.
Yes, all benzodiazepines carry a risk of addiction. However, the potential for dependence can vary based on how quickly a medication acts and how long its effects last. Drugs with a rapid onset, such as Xanax, often have a higher potential for misuse because the immediate calming effect can reinforce a pattern of repeated use. Research confirms that both short-acting and long-acting benzodiazepines can cause dependence when used for extended periods.
Short-acting benzos (like Xanax and Ativan) provide fast relief but also wear off quickly, which can lead to more frequent dosing and a higher risk of dependence.
Long-acting benzos (like Valium and Klonopin) remain in the body longer, but physical dependence still develops with prolonged use.
Even when taken exactly as prescribed, long-term use increases the risk of addiction. For this reason, healthcare providers typically recommend benzodiazepines for short-term use only and monitor their patients closely.
The signs of benzodiazepine addiction involve a combination of behavioral changes and physical symptoms. An individual might begin taking larger doses than prescribed, become preoccupied with obtaining their next dose, or engage in “doctor shopping” to get multiple prescriptions. As physical dependence develops, withdrawal symptoms will appear if the medication is stopped or the dose is reduced.
Common signs and symptoms include:
Memory problems or frequent confusion
Persistent drowsiness or sedation
Slurred speech and poor coordination
Unexplained mood swings, irritability, or depression
Needing more of the drug to feel the same effect
Experiencing withdrawal symptoms like anxiety, sweating, tremors, or seizures when the drug is not taken
Studies indicate that the misuse of benzodiazepines is a growing public health concern, with an increasing number of emergency room visits linked to their use. These risks underscore the importance of professional help from benzodiazepine detox centers or rehab facilities [2]. A key warning sign is when a person’s daily functioning—at work, school, or in relationships—begins to decline due to their drug use.
It’s time to look for benzodiazepine addiction treatment when you find it difficult to stop or cut back due to withdrawal symptoms or strong cravings. If you’re continuing to use despite experiencing negative effects on your health, relationships, or daily life, it’s a clear sign that you need professional help.
Doctors emphasize that quitting benzodiazepines “cold turkey” can be extremely risky. Withdrawal can lead to severe insomnia, panic attacks, hallucinations, and even life-threatening seizures. Therefore, detox should always be managed by gradually reducing the dose under medical supervision.
You should think about reaching out for professional assistance if you:
Have been using benzodiazepines for more than a few weeks without medical advice.
Have increased the dosage on your own.
Mix benzodiazepines with other substances, such as alcohol or opioids, which significantly heightens the risk of a fatal overdose.
Suffer from withdrawal symptoms if you miss a dose.
Notice that your relationships, job, or daily responsibilities are taking a hit due to your use.
Stopping benzodiazepines abruptly can be life-threatening. These medications alter brain chemistry, and when they are suddenly removed, the central nervous system can rebound with severe and dangerous withdrawal symptoms.
Some of the most serious risks of unsupervised withdrawal include:
Seizures: Abruptly stopping can trigger grand mal seizures, even in individuals with no prior history of them.
Hallucinations and Delirium: The brain’s sudden readjustment can cause profound confusion, paranoia, or psychosis.
Severe Rebound Anxiety and Panic: Withdrawal often causes a return of anxiety or insomnia that is far more intense than the original condition.
Dangerous Vital Sign Changes: Rapid increases in heart rate, blood pressure, and body temperature can place extreme stress on the body.
Due to these risks, a gradual, medically supervised taper is the only safe way to stop using benzodiazepines. This process is best managed in a professional treatment setting [3].
Benzodiazepine addiction treatment involves several critical stages: medical detoxification, behavioral therapies, and ongoing recovery support. This comprehensive approach targets both the physical and psychological aspects of addiction.
1. Medical Detoxification
The treatment begins with medically supervised detoxification, essential due to the risks of sudden withdrawal. In a specialized detox facility, healthcare professionals gradually taper the dosage while monitoring the patient to minimize withdrawal symptoms and prevent serious complications, such as seizures.
2. Behavioral Therapies
After detox, individuals engage in structured behavioral therapy at rehabilitation centers. These therapies, including Cognitive Behavioral Therapy (CBT), help identify psychological triggers and develop healthier coping strategies. Sessions may occur individually or in groups, fostering a supportive community.
3. Support Systems and Long-Term Recovery
Long-term recovery relies heavily on ongoing support. Treatment programs often include family therapy, group sessions, and peer support networks. These resources help individuals maintain sobriety and provide continuous emotional and medical support as they transition back to everyday life.
Through this integrated approach, patients are equipped with the tools and support necessary for lasting recovery [4].
The duration of benzodiazepine addiction treatment is highly individualized. It depends on factors like the severity of the dependence, the specific type of benzodiazepine used, and the presence of any co-occurring mental health conditions. While some may complete a program in a few weeks, others require several months of care [5].
Detox Phase: The initial detox and stabilization phase typically takes one to four weeks. Short-acting benzos like Xanax may have a faster but more intense withdrawal, while long-acting benzos like Valium require a longer, more gradual taper.
Inpatient or Outpatient Programs: Inpatient rehab programs usually last from 30 to 90 days. Outpatient programs can extend for a longer period but offer more flexibility.
Aftercare: Recovery is an ongoing process. Aftercare, including continued therapy and support groups, is often recommended for months or even years to prevent relapse and maintain stability.
Overall, the timeline for benzo treatment is individualized. While detox is relatively short, the full rehabilitation journey can take months, with long-term management to prevent relapse.
Successful recovery extends beyond the initial treatment phase. Long-term sobriety depends on developing effective relapse prevention strategies to manage cravings and stress.
Core components of relapse prevention include:
Coping Skills Training: Learning healthy ways to manage anxiety, stress, or insomnia without medication through techniques like mindfulness and relaxation exercises.
Ongoing Therapy: Continuing with individual or group therapy to address the underlying issues that contributed to the addiction.
Peer Support: Engaging with support groups provides encouragement, accountability, and a community of people who understand the recovery journey.
Long-Term Care and Monitoring: Regular check-ins with healthcare providers help track progress and ensure continued stability.
Benzodiazepine misuse is a significant public health issue. Data reveals a concerning trend of increasing dependence and misuse, particularly when these medications are used long-term or without close medical supervision.
Prevalence of Use: An estimated 12.6% of U.S. adults report using benzodiazepines, with about 17% of those individuals misusing the drug.
Addiction and Misuse Rates: Misuse is most common among people who are self-medicating for sleep issues or mental health conditions. Combining benzodiazepines with opioids or alcohol dramatically increases the risk of a fatal overdose.
Overdose Data: Between 1996 and 2013, the number of overdose deaths involving benzodiazepines increased more than fourfold. The majority of these fatal overdoses also involved opioids [6].
Benzodiazepines are frequently prescribed to alleviate the symptoms of various mental health conditions, including anxiety, panic disorders, and insomnia. These medications can provide significant short-term relief, creating a sense of calm and stability.
However, the long-term use of benzodiazepines presents a double-edged sword; it may exacerbate psychiatric symptoms, leading to increased emotional instability and dependency. Given their profound impact on mental health, healthcare providers must prescribe these medications judiciously, accompanied by meticulous monitoring to promote safe and effective treatment outcomes.
1. Common Prescriptions
Benzodiazepines are utilized in the treatment of an array of mental health issues, including generalized anxiety disorder, panic disorder, chronic insomnia, epilepsy, and, in certain cases, managing the withdrawal symptoms from alcohol.
Among the most commonly prescribed benzodiazepines are diazepam, lorazepam, alprazolam, and clonazepam, each varying in its potency and duration of action, catering to the specific needs of patients.
2. Impact on Mental Health
While these medications can be effective in the short term, their prolonged use can lead to a troubling cycle of dependence, potentially aggravating mood disorders in the process.
Chronic users of benzodiazepines often experience a range of adverse effects, including depression, cognitive impairment, and a significantly heightened risk of suicidal thoughts and behaviors.
3. Dual Diagnosis Concerns
A considerable number of patients in benzodiazepine treatment centers are grappling with dual diagnoses, where substance use disorders coexist with mental health conditions.
To facilitate a successful recovery, it is important to address both the addiction to benzodiazepines and the underlying mental health issues simultaneously [7].
Though benzodiazepines are frequently prescribed for various mental health disorders, their misuse or extended use can lead to additional psychiatric complications. Therefore, effective treatment for benzodiazepine addiction must encompass both the addictive properties of these medications and the intricacies of the underlying mental health challenges faced by individuals.
How do you treat benzodiazepine addiction?
Treatment involves a multi-faceted approach, starting with a medically supervised detox to safely taper off the drug. This is followed by behavioral therapies like CBT, counseling, and long-term support through aftercare planning to prevent relapse.
What medication is used for benzo withdrawals?
A slow taper using a long-acting benzodiazepine, such as diazepam (Valium), is the most common method to reduce the severity of withdrawal. Other medications may be used to manage specific symptoms. This process must always be supervised by a medical professional.
What is the antidote for benzodiazepine addiction?
Flumazenil is an antidote used in emergencies to reverse an acute benzodiazepine overdose, but it is not a treatment for addiction. Long-term addiction requires a comprehensive treatment plan focused on gradual tapering, therapy, and support.
What does a benzo addiction look like?
Signs of addiction include a growing tolerance (needing more for the same effect), intense cravings, and difficulty functioning without the drug. Other common signs are drowsiness, memory issues, mood swings, and neglecting responsibilities.
What helps benzo recovery?
Successful recovery is built on a foundation of medical care, psychological therapy, and a strong support network. A gradual, supervised taper prevents dangerous withdrawal. Therapy helps develop coping skills, and support groups provide a sense of community.
At District Behavioral Health, we provide compassionate, evidence-based care to help individuals safely overcome benzodiazepine dependence. Our specialized treatment programs combine medical expertise, counseling, and long-term support so you don’t have to face recovery alone.
Our comprehensive programming includes:
Medication-Assisted Detox: Safe, medically supervised tapering to reduce withdrawal risks.
Crisis Intervention & Stabilization: Immediate care to restore safety and stability during difficult moments.
Inpatient & Residential Programs: 24/7 structured care with therapy, medical oversight, and a healing environment.
Partial Hospitalization Programs (PHP): Full-day treatment offering intensive therapy without overnight stays.
Intensive Outpatient Programs (IOP): Flexible treatment that balances recovery with work, school, or family responsibilities.
Outpatient Programs (OP): Ongoing therapy and support designed for long-term recovery.
If you or a loved one is struggling with benzodiazepine addiction, professional help is just a call away. Reach out to our caring team today at (888) 707-6073 to begin your path toward recovery.
[1]. https://www.drugs.com/article/benzodiazepines
[2]. https://pmc.ncbi.nlm.nih.gov/articles/PMC4657308/
[3]. https://www.nejm.org/doi/full/10.1056/NEJMra1611832
[4]. https://pubmed.ncbi.nlm.nih.gov/30554562/
[5]. https://pubmed.ncbi.nlm.nih.gov/31121495/
[6]. https://pmc.ncbi.nlm.nih.gov/articles/PMC6007645/
[7]. https://pmc.ncbi.nlm.nih.gov/articles/PMC8629021/
Check out our addiction recovery blog to learn more about substance use disorders and how to get effective treatment.

We strive to provide a comfortable, home-like environment during your recovery journey. Browse our facility images below to take a look at our upscale residential facilities.
Paying Out Of Pocket without Insurance
If you can’t pay your co-pay amount
Paying Out Of Pocket with Insurance
(Depending on insurance plan)
View our wide selection of accepted providers. Don’t see yours? Call our admissions team for help.











Whether you’re seeking help for yourself or a loved one, our admissions team is available 24/7 to answer your questions and guide you toward the right care.

| March | 2026 | |||||
|---|---|---|---|---|---|---|
| March 2026 | ||||||
| SSunday | MMonday | TTuesday | WWednesday | TThursday | FFriday | SSaturday |