Home
Locations 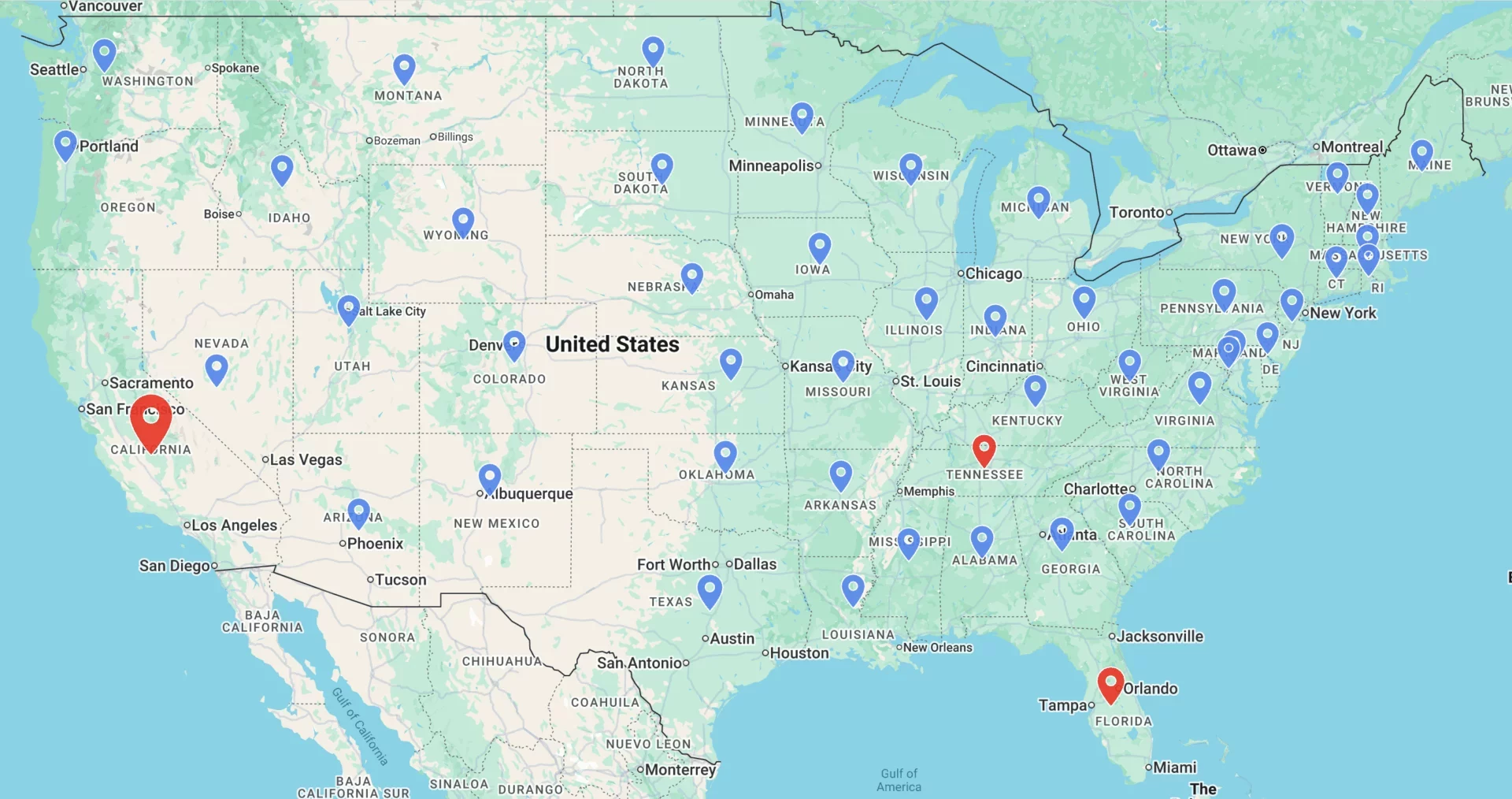
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions

Home
Locations 
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions








Matthew D'Ursov

Amy Leifeste

Karena Mathis



Addiction and mental health challenges often influence the way thoughts, emotions, and decisions are processed each day. For many, the idea of stepping away from daily responsibilities to seek care feels overwhelming. CBT Therapy is designed to meet individuals where they are, providing structured therapeutic support that fits into real schedules. It helps people address underlying patterns without disconnecting from work, family, or daily routines.
District Behavioral Health delivers CBT Therapy through the Renaissance Recovery network. These outpatient programs focus on evidence-based therapy, emotional regulation, and practical skill development without requiring residential care. This flexible structure supports long-term wellness by helping individuals strengthen coping abilities while staying connected to everyday life.
See more about our CBT Therapy program below.
Our behavioral health services support men and women struggling with substance use and co-occurring mental health disorders. District Behavioral Health focuses on providing a comprehensive continuum of care, including personalized outpatient treatment, intensive outpatient (IOP) and partial hospitalization programs (PHP), and coordinated support services designed to help individuals stabilize, develop effective coping skills, and build lasting recovery within their communities.
Cognitive Behavioral Therapy (CBT) helps individuals shift their reactions by first identifying and reshaping distorted beliefs. This structured approach trains the mind to respond to stress more clearly and reduce harmful patterns over time.
At District Behavioral Health (DBH), CBT is integrated into personalized treatment plans. Our interventions focus on symptom relief, long-term stability, and lasting emotional control, ensuring clients gain both immediate support and lifelong coping strategies.
This blog outlines how CBT works, what conditions it treats, and how individuals benefit from behavioral therapy techniques at DBH.
CBT is a structured, evidence-based form of psychotherapy built on the principle that our belief systems shape our emotional responses [1]. When those beliefs become distorted, they can trigger actions that increase stress or disrupt daily functioning.
CBT works by:
Identifying unhelpful thought patterns that fuel distress.
Challenging and reshaping those beliefs into more balanced perspectives.
Introducing practical tools that reduce reactivity and support healthier choices.
Over time, these changes help lower symptoms, restore internal control, and build emotional resilience.
What to Expect in CBT Sessions
CBT sessions follow a structured format. Each session has a defined goal, and progress is measured along the way.
Most clients begin CBT to address anxiety or depression, but the therapy is effective across a wide range of conditions tied to thinking and behavior.
Clients learn to observe their thoughts, test their accuracy, and apply new techniques that shift how they respond to challenges.
Through repetition, these strategies reduce impulsive behaviors and strengthen emotional judgment.
The result is not just symptom relief, but the development of lifelong skills that support healthier thinking, improved decision-making, and greater stability.
For many individuals, CBT helps reduce distress by teaching strategies that build self-awareness and improve the ability to respond with stability. It is one of the most versatile therapies, applied across a wide range of mental health and behavioral conditions.
The most common conditions treated with CBT include:
Eating Disorders
Eating disorders often develop around distorted beliefs about food, appearance, and control. These patterns create rituals that reinforce guilt, restriction, or bingeing. CBT works to break this cycle by restoring structure to eating habits and challenging perfectionistic thinking. Over time, clients replace rigid, self-critical beliefs with a more balanced and compassionate view of themselves. [2]
Major Depressive Disorder
In depression, negative belief patterns fuel low mood and loss of interest. CBT helps identify and challenge these internal narratives—such as self-blame or hopelessness—that sustain inactivity. Therapists gradually introduce behavioral tasks to increase daily structure and energy. As these changes are repeated, motivation improves and symptoms lift in measurable ways.
Panic Disorder
Panic disorder involves sudden episodes of intense fear, often accompanied by symptoms such as shortness of breath, chest tightness, or a racing heart. CBT targets the thought process that turns normal physical sensations into perceived danger. Through gradual exposure to feared sensations, clients reduce sensitivity and learn to prevent escalation into full panic attacks.
Social Anxiety
Social anxiety is marked by fear of being judged, watched, or rejected in everyday interactions. This often leads to avoidance. CBT breaks the cycle by addressing the internal story behind the fear. Clients practice small, structured tasks—such as speaking in groups or initiating conversations. With repetition, discomfort decreases and confidence grows in social settings.
Post-Traumatic Stress Disorder (PTSD)
Trauma can leave behind avoidance behaviors and distorted beliefs tied to the event. CBT for PTSD provides structure to recovery by mapping these patterns and gradually introducing exposure work, supported by calming techniques. As clients process their trauma in a safe, controlled way, symptoms ease and a sense of internal control returns. [3]
Obsessive-Compulsive Disorder (OCD)
OCD traps individuals in a cycle of intrusive thoughts and compulsive rituals (for example, repeated handwashing). While rituals provide short-term relief, they reinforce distress over time. CBT uses Exposure and Response Prevention (ERP) to break this loop. Clients face triggers directly without performing the ritual, and with practice, the urge weakens and anxiety decreases.
Phobias
Phobias trigger intense, automatic fear tied to specific objects or situations, leading to avoidance. CBT targets both the fear and the avoidance behavior. Through graded exposure, clients face the feared object or activity in controlled steps that match their tolerance. Repetition helps reduce fear and restore normal functioning.
Sleep Disturbances
Sleep problems often stem from unhelpful thoughts and routines that disrupt rest. CBT for Insomnia (CBT-I) addresses both behavior and mindset. Clients establish steady sleep habits, challenge anxious thoughts about rest, and learn relaxation techniques. Over time, the body resets its natural sleep cycle.
Generalized Anxiety Disorder
GAD involves persistent, excessive worry that feels difficult to control. CBT helps clients distinguish between the process of worrying and the actual content of their thoughts. By testing anxious predictions, reducing avoidance, and practicing controlled exposure to fears, clients slow mental overactivity and regain emotional steadiness. [4]
When looking for a qualified CBT therapist, it’s essential to review their credentials, training, and approach to structured care.
At District Behavioral Health (DBH), all providers trained in cognitive therapy have extensive experience applying CBT interventions across multiple conditions [5]. This ensures that treatment is both evidence-based and tailored to the individual.
CBT therapists receive advanced training in:
Identifying distorted thought processes
Developing action plans tailored to each client’s symptoms and personal goals
Using structured methods that track progress and outcomes
CBT begins by identifying the patterns of thought and behavior that increase stress or lead to avoidance. Once these patterns are clear, clients learn to test them, challenge them, and develop healthier responses that withstand pressure [6].
Each session typically includes:
Targeted education about the connection between thoughts, feelings, and behaviors
Structured tasks and exercises designed to practice new skills
Feedback and progress tracking tied to real-life outcomes
These steps are repeated until new habits take hold and symptoms begin to shift.
Assessment and goal setting – Identifying challenges and defining therapy goals
Thought monitoring and restructuring – Recognizing and reframing distorted thinking
Behavioral experiments – Testing new ways of responding in real-life situations
CBT exercises – Homework such as journaling, thought records, or relaxation training
Skill building – Strengthening coping strategies and problem-solving abilities
Maintenance and review – Reinforcing progress and preventing relapse
Why CBT Works
CBT is not about “venting” but about training the mind. Its structured approach allows clients to:
Track measurable changes
Understand the link between thoughts, emotions, and behaviors
Build practical skills that last long after therapy ends
Each model of CBT is built on the same foundational principle: thoughts, feelings, and behaviors are interconnected. By changing unhelpful thought patterns, individuals can improve emotional well-being and make healthier choices. Different CBT approaches apply these principles in unique ways to match specific conditions [7].
Traditional CBT focuses on how thoughts and behaviors reinforce one another. The process begins by identifying the beliefs that drive emotional and behavioral reactions. Clients track these patterns and practice new habits that reduce symptoms. Sessions are structured, goal-oriented, and emphasize what can be changed in the present to improve functioning.
MBCT integrates mindfulness practices with traditional CBT techniques. Originally developed to reduce relapse in people with recurrent depression, MBCT teaches clients to observe thoughts without reacting to them. This skill interrupts the cycle of rumination before it escalates, helping individuals maintain stability and prevent relapse.
Exposure and Response Prevention (ERP)
ERP is a specialized form of CBT most often used for obsessive-compulsive disorder (OCD) and phobias. Clients identify the thoughts, images, or situations that trigger anxiety and then face them directly—without engaging in the usual ritual or avoidance behavior. Over time, repeated exposure reduces anxiety and weakens the urge to perform compulsions.
TF-CBT is designed for individuals with post-traumatic stress disorder (PTSD) or trauma experienced early in life. It combines cognitive restructuring with gradual exposure to traumatic memories. Clients process the event in manageable steps while building coping skills to regulate fear and remain grounded in the present. This approach helps reduce trauma symptoms and restore a sense of safety.
DBT was developed for people who experience intense mood swings, self-destructive behaviors, or unstable relationships. While rooted in CBT principles, DBT emphasizes acceptance alongside change. Clients practice skills in small, structured steps and apply them between sessions to reinforce their learning.
DBT focuses on four core skill areas:
Emotional regulation – managing intense feelings without becoming overwhelmed
Distress tolerance – coping with crises in healthier ways
Mindfulness – staying present and aware without judgment
Interpersonal effectiveness – improving communication and building stable relationships
CBT is beneficial but is not the right fit for every situation [8]. Understanding both its strengths and limitations can help determine whether it’s the right approach for an individual’s needs.
CBT is widely considered a first-line treatment across many mental health settings because it offers clear structure, measurable progress, and lasting skills.
From the outset, CBT outlines a plan with clearly defined goals. Each session builds toward these goals, and progress is monitored throughout. This clarity helps both client and therapist see what’s working and what still needs attention.
CBT is one of the most researched therapies, with strong evidence for conditions such as depression, anxiety, and OCD. Its tools are grounded in science rather than trial and error, making it a reliable choice in settings where outcomes matter.
Most CBT treatment plans last between 12 and 20 sessions, although some people notice improvements sooner. The structured format helps keep therapy on track, while the skills learned often continue to benefit clients long after treatment ends, reducing the risk of relapse.
Builds Lifelong Skills
CBT equips clients with practical tools—such as thought-challenging, problem-solving, and stress management—that can be applied independently in daily life. These skills promote resilience and long-term stability.
While CBT is highly effective, it may not be the best fit for everyone. Some limitations include:
Success in CBT depends on consistent effort outside of sessions. Clients are expected to complete homework, track thoughts, and practice new skills. For some, this level of commitment can be demanding, especially in the early stages.
CBT can be challenging for individuals with significant memory, attention, or learning difficulties. In such cases, tasks may need to be simplified, shortened, or repeated more often to be effective.
CBT focuses primarily on present thoughts and behaviors rather than exploring deep-rooted issues from the past. Clients seeking an in-depth exploration of early experiences or unconscious processes may find CBT less satisfying compared to other therapeutic approaches.
The length of CBT depends on the condition being treated, the severity of symptoms, and the individual’s pace of progress.
On average:
Most CBT treatment plans last between 12 and 24 sessions, whether in-person or online [9].
Research indicates that many individuals typically begin to see improvement within approximately 16 sessions.
For long-term or complex conditions—such as PTSD, OCD, or trauma linked to early life experiences—therapy may take longer. Some clients need additional time to work through exposure tasks or to build skills gradually.
In some instances, therapy may continue for several months, with booster sessions scheduled later to maintain progress and prevent relapse.
The key strength of CBT is that it equips clients with practical skills they can continue using independently, even long after formal sessions have ended.
CBT is most effective when started early—before symptoms become overwhelming. If your mental health challenges begin to interfere with daily functioning, relationships, or overall well-being, it may be time to seek help.
Many people delay treatment, hoping things will improve on their own. Unfortunately, without support, unhelpful patterns often become stronger.
Signs it may be time to consider CBT:
Anxiety or depression lasting more than two weeks
Fear, guilt, or worry making daily tasks harder
Noticeable changes in sleep, appetite, or energy without a clear cause
Past trauma repeatedly resurfacing and shaping your choices
Avoiding people, places, or activities because of fear or anxiety
CBT for anxiety involves identifying fear-based thoughts and challenging them through exposure or logic. Behavioral experiments help reduce avoidance. Techniques like thought journaling, exposure tasks, and relaxation skills support daily practice.
The five steps include:
1. Identify the problem
2. Recognize automatic thoughts.
3. Evaluate thought patterns
4. Develop alternative responses
5. Practice new behaviors without fail
A person with panic disorder might start by tracking when and where the panic begins. They learn how to slow their breathing and stay present during early signs. Gradual exposure to avoided places is added as confidence builds. Progress is reviewed in each session to guide the next step.
CBT teaches skills that target different parts of the cycle. These include thought testing, breathing control, activity scheduling, and exposure. Clients also learn how to track patterns and notice changes as they happen.
Most insurance plans include CBT under mental health coverage. Benefits depend on your provider, diagnosis, and the terms of your policy.
At District Behavioral Health Group, we offer evidence-based cognitive behavioral therapy (CBT) to help individuals manage mental health disorders and substance use challenges.
CBT focuses on identifying and changing unhelpful thought patterns and behaviors, providing patients with practical skills to regain control, reduce symptoms, and build long-term stability. Our nationwide recovery network ensures a clear, connected treatment path every step of the way.
Our comprehensive programming includes:
Medication-Assisted Detox: Safe, medically supervised detox when substance use co-occurs with mental health issues.
Crisis Intervention & Stabilization: Immediate support to restore safety and stability.
Inpatient & Residential Programs: 24/7 live-in care with therapy, medical support, and structured daily routines.
Partial Hospitalization Programs (PHP): Full-day treatment without overnight stays, offering intensive therapy.
Intensive Outpatient Programs (IOP): Part-time therapy that provides structure while balancing daily life.
Outpatient Programs (OP): Flexible therapy sessions to maintain recovery and independence.
If you or a loved one is seeking CBT therapy as part of recovery, call our caring team today at (888) 707-6073 to begin treatment.
[1] https://www.ncbi.nlm.nih.gov/books/NBK279297/
[2] https://www.bbwpublisher.com/index.php/ssr/article/view/8443
[3] https://www.tandfonline.com/doi/full/10.1080/0145935X.2024.2340550
[4] https://jamanetwork.com/journals/jamapsychiatry/fullarticle/2810866
[5] https://www.tandfonline.com/doi/full/10.1080/15374416.2017.1381914
[6] https://link.springer.com/chapter/10.1007/978-1-4615-0567-9_21
[7]https://journals.lww.com/jonmd/abstract/2021/11000/the_effectiveness_of_cognitive_behavioral_therapy.9.aspx
[8] https://pmc.ncbi.nlm.nih.gov/articles/PMC9840507/
[9] https://pmc.ncbi.nlm.nih.gov/articles/PMC3390320/
Check out our addiction recovery blog to learn more about substance use disorders and how to get effective treatment.

We strive to provide a comfortable, home-like environment during your recovery journey. Browse our facility images below to take a look at our upscale residential facilities.
Paying Out Of Pocket without Insurance
If you can’t pay your co-pay amount
Paying Out Of Pocket with Insurance
(Depending on insurance plan)
View our wide selection of accepted providers. Don’t see yours? Call our admissions team for help.











Whether you’re seeking help for yourself or a loved one, our admissions team is available 24/7 to answer your questions and guide you toward the right care.

| March | 2026 | |||||
|---|---|---|---|---|---|---|
| March 2026 | ||||||
| SSunday | MMonday | TTuesday | WWednesday | TThursday | FFriday | SSaturday |