Home
Locations 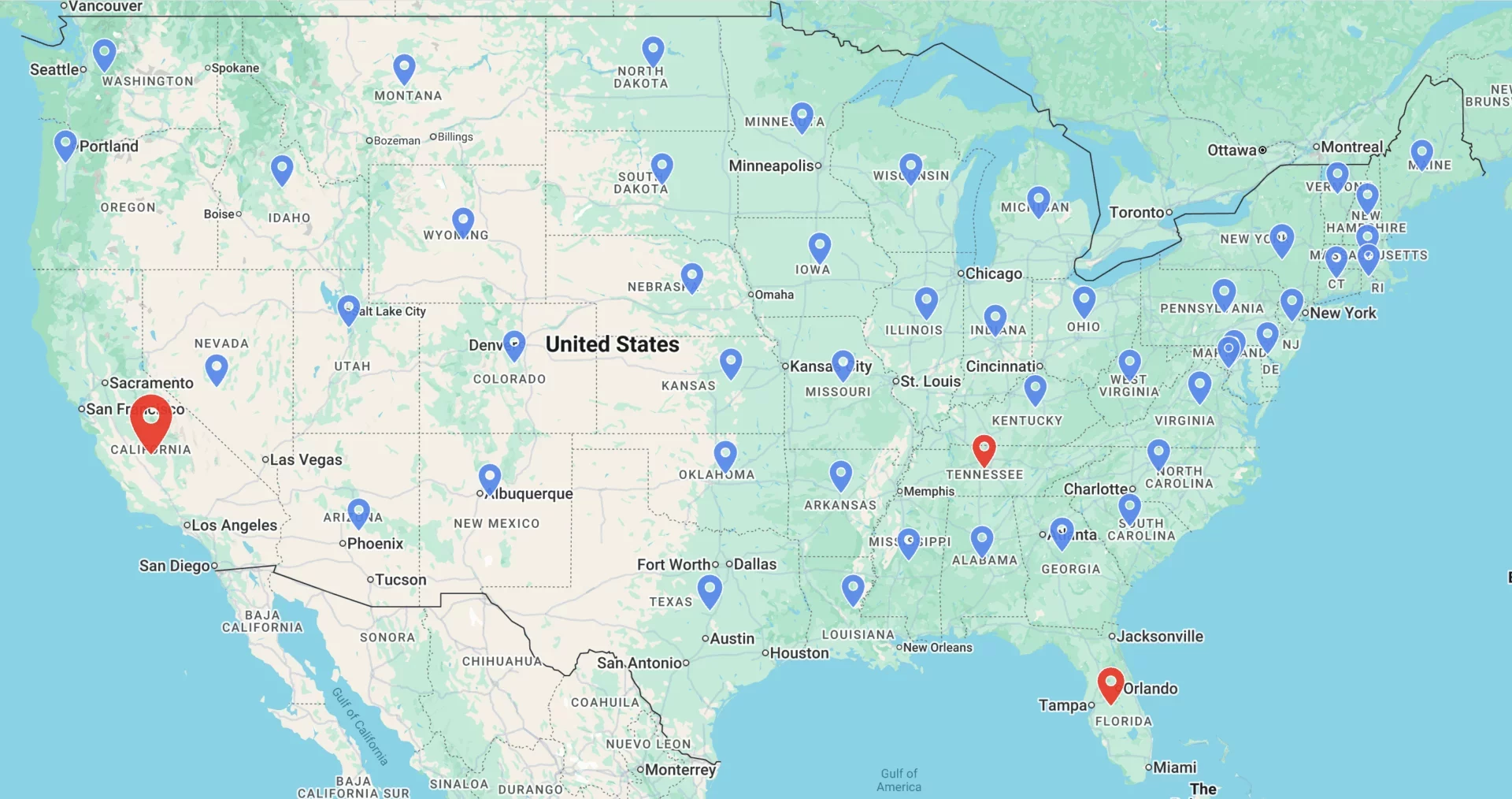
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions

Home
Locations 
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions








Matthew D'Ursov

Amy Leifeste

Karena Mathis



Individuals seeking Dialectical Behavior Therapy (DBT) often struggle with intense emotional swings and “all-or-nothing” thinking that can strain even the closest relationships. Many feel exhausted by a cycle of impulsive reactions and may feel that traditional talk therapy hasn’t provided the concrete “how-to” tools needed to navigate a crisis without making it worse. The primary hurdle is the gap between wanting to change and having the actual skills to regulate distress in real-time.
Our DBT program uses a structured, evidence-based approach that focuses on teaching practical skills for emotional regulation, distress tolerance, mindfulness, and interpersonal effectiveness. Care is delivered through clinician-led sessions and skills-focused therapeutic support.
This skills-driven model helps individuals move beyond crisis management and build long-term emotional stability and confidence.
Learn more about DBT therapy options available through Renaissance Recovery and Gratitude Lodge below.
Our behavioral health services support men and women struggling with substance use and co-occurring mental health disorders. District Behavioral Health focuses on providing a comprehensive continuum of care, including personalized outpatient treatment, intensive outpatient (IOP) and partial hospitalization programs (PHP), and coordinated support services designed to help individuals stabilize, develop effective coping skills, and build lasting recovery within their communities.
Dialectical Behavior Therapy (DBT) is an evidence-based psychotherapy designed to help individuals manage intense emotions, reduce harmful behaviors, and improve relationships. At District Behavioral Health (DBH), DBT is integrated into personalized treatment plans to support clients facing emotional dysregulation, self-destructive patterns, and interpersonal challenges.
Combining principles from Cognitive Behavioral Therapy (CBT) with mindfulness practices, DBT emphasizes both acceptance and change—helping individuals build resilience and lead more fulfilling lives.
This blog will explain what DBT is, the core skills it teaches, and how these skills are applied in treatment.
DBT is a structured, skills-based therapy that teaches individuals how to manage overwhelming emotions and modify behaviors that interfere with their daily life. According to the Minnesota Department of Human Services, DBT balances acceptance strategies (validating a person’s experience) with change strategies (developing new coping skills) to improve overall functioning.
Initially developed for borderline personality disorder, DBT is now widely used to treat:
Suicidal thoughts and self-harm
Eating disorders
Substance use disorders
Post-traumatic stress disorder (PTSD)
Mood instability and impulsivity
Its primary goal is to reduce life-threatening behaviors while building long-term emotional and behavioral stability.
As outlined by the Administration for Children and Families, DBT typically includes:
Individual therapy – focused on personal goals and skill application
Group skills training – teaching core DBT skills in a supportive setting
Phone coaching – offering real-time support between sessions
At DBH, DBT is more than crisis management—it’s a comprehensive therapeutic approach that helps clients regulate emotions, strengthen relationships, and build a life worth living. [1]
Research published in the Journal of Psychiatric Practice confirms DBT as one of the most thoroughly studied therapies for complex mental health conditions. Its dual focus on validation and change helps clients feel understood while empowering them to take control of their emotional responses.
DBT is built around four core skill areas, each designed to help individuals navigate life more effectively. These skills are taught in group sessions and practiced in daily life, making them highly practical and transformative.
Mindfulness enables individuals to stay present and observe their thoughts and emotions without judgment. According to the Association for Behavioral and Cognitive Therapies, mindfulness enhances awareness of internal experiences, enabling more intentional and balanced responses.
Key components:
Observing thoughts, feelings, and sensations as they arise
Describing experiences without labeling them as “good” or “bad”
Participating fully in the present moment
Mindfulness lays the foundation for all other DBT skills. [2]
Distress tolerance skills help individuals survive emotional crises without worsening the situation. These techniques are handy for managing urges toward self-harm or impulsive behavior.
Core strategies:
Distraction – shifting focus through engaging activities
Self-soothing – calming the body using sensory input
Radical acceptance – acknowledging reality, even when painful
These tools allow individuals to endure difficult emotions until they pass, reducing the risk of reactive behaviors.
Emotion regulation teaches clients how to understand and manage strong emotions before they escalate. Research shows that emotional dysregulation often leads to mood swings, anger, or sadness that feel uncontrollable.
Key techniques:
Identifying and labeling emotions accurately
Reducing vulnerability through physical health and self-care
Increasing positive emotions through enjoyable activities
Applying opposite actions (e.g., approaching instead of avoiding fear triggers)
These strategies help individuals respond to emotions with clarity and control.
Interpersonal effectiveness skills improve communication, boundary-setting, and relationship stability. This area focuses on striking a balance between self-respect, relationship goals, and personal needs.
Essential skills:
Asking for needs clearly and respectfully
Saying no without guilt
Resolving conflicts while maintaining self-esteem
Strengthening connections with supportive people
These skills are especially valuable for individuals who struggle with unstable or conflict-driven relationships.
Dialectical Behavior Therapy (DBT) is a structured, evidence-based approach that helps individuals manage overwhelming emotions, reduce harmful behaviors, and build healthier relationships. It combines individual therapy, group skills training, and ongoing support to teach practical coping strategies that can be applied in everyday life. By balancing acceptance with change, DBT empowers clients to create greater emotional stability and personal control. [3]
DBT is built on a four-part framework designed to provide comprehensive, consistent support:
Individual therapy – Focuses on personal goals, motivation, and reducing self-destructive behaviors.
Group skills training – Teaches DBT core skills in a supportive, interactive setting.
Phone coaching – Offers real-time guidance during emotional crises or high-stress situations.
Consultation teams – Support therapists in maintaining treatment quality and consistency.
This structure ensures that clients receive both personalized care and practical tools they can apply in their daily lives.
The heart of DBT lies in its dialectical philosophy—the balance between accepting current struggles and working toward meaningful change. Therapists validate clients’ emotional experiences while encouraging them to adopt new strategies for healthier behavior.
Key therapeutic goals include:
Building mindfulness to stay grounded in the present moment
Tolerating distress without resorting to harmful actions
Regulating emotions before they escalate
Improving communication and maintaining stable relationships
According to research published in the Journal of Psychiatric Practice, DBT is rooted in cognitive-behavioral therapy principles but expands them by integrating mindfulness and acceptance strategies. Unlike traditional CBT, which focuses primarily on thought patterns, DBT emphasizes both emotional acceptance and behavioral change.
This dual focus is especially effective for individuals with emotional dysregulation, enabling them to develop a step-by-step approach for managing intense feelings and preventing reactive behaviors.
DBT skills are taught systematically in four modules:
Mindfulness – Enhances awareness and reduces impulsivity
Distress Tolerance – Builds tools to survive emotional crises
Emotion Regulation – Helps manage and stabilize mood
Interpersonal Effectiveness – Strengthens communication and relationship skills
As highlighted by the Association for Behavioral and Cognitive Therapies, these modules provide a clear roadmap for clients to practice strategies, track progress, and build confidence. By combining therapy with real-life application, DBT ensures that clients not only learn the skills but also integrate them into lasting habits. [4]
Dialectical Behavior Therapy (DBT) is a specialized, evidence-based treatment designed to help individuals who struggle with intense emotions, self-destructive behaviors, and unstable relationships. Originally developed for borderline personality disorder, DBT has since been adapted to treat a wide range of mental health conditions. By focusing on emotional regulation, distress tolerance, mindfulness, and interpersonal effectiveness, DBT equips clients with practical tools to manage challenges and improve overall quality of life.
DBT is especially effective for individuals experiencing:
Borderline personality disorder
Suicidal ideation and self-injury
Eating disorders (e.g., bulimia, binge eating)
Substance use disorders
Post-traumatic stress disorder (PTSD)
Its structured approach helps reduce life-threatening behaviors while promoting emotional stability and healthier coping mechanisms.
According to the ACF Prevention Services database, DBT is also used with adolescents and families dealing with emotional instability, behavioral risk, or interpersonal conflict. This demonstrates DBT’s versatility across different populations.
For young people, DBT offers skills to:
Manage strong emotions
Improve peer and family relationships
Reduce impulsivity and reactive behaviors
DBT’s adaptability makes it a valuable resource in both individual and family-based treatment settings.
Studies published on PubMed Central highlight DBT’s effectiveness in treating a variety of psychiatric conditions—particularly those involving self-harm, mood instability, and trauma. Clinicians have successfully applied DBT strategies to:
Mood disorders (e.g., depression, bipolar disorder)
Trauma-related conditions
Certain personality disorders beyond borderline
Because DBT balances acceptance and change, it can be tailored to meet diverse clinical needs, making it one of the most flexible and impactful therapies available.
The Association for Behavioral and Cognitive Therapies (ABCT) emphasizes the importance of DBT group therapy in fostering a supportive community environment.
In group sessions, clients:
Practice new skills
Share experiences
Learn from others facing similar challenges
This peer-supported model reinforces accountability, builds connection, and enhances motivation—making it a vital component of DBT treatment. [5]
Dialectical Behavior Therapy (DBT) is widely recognized for its effectiveness in treating individuals with emotional dysregulation, self-destructive behaviors, and complex mental health conditions. Its structured, skills-based approach offers both immediate symptom relief and long-term resilience.
Clinical Effectiveness
DBT has been clinically proven to:
Reduce suicidal behaviors and self-injury
Improve emotional regulation
Enhance overall psychological functioning
A clinical review found that individuals receiving DBT experienced fewer psychiatric hospitalizations and reported a higher quality of life compared to those receiving standard treatment. DBT helps clients replace harmful coping strategies—such as self-harm—with healthier alternatives like distress tolerance techniques, allowing them to manage crises more safely and effectively.
According to a study published in Frontiers in Psychology, DBT offers sustained improvements over time, including:
Greater emotional stability
Stronger social relationships
Lower relapse rates for conditions such as substance misuse and eating disorders
The therapy’s structured skill modules—mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness—can be practiced long after formal treatment ends, contributing to lasting behavioral change. [6]
DBT is adaptable across age groups and clinical presentations:
Adolescents – Helps manage mood swings, reduce impulsivity, and improve family communication
Adults with borderline personality disorder – Reduces suicide attempts and self-injurious behaviors
Individuals with trauma histories – Supports emotional regulation and distress processing without re-traumatization
This flexibility makes DBT a valuable option in both individual and group therapy settings.
The success of DBT lies in its comprehensive and balanced design. It integrates:
Individual therapy for personalized support
Group skills training for peer learning and practice
Ongoing coaching and consultation for real-time guidance
By combining acceptance (validating current struggles) with change (building new coping strategies), DBT fosters emotional resilience and empowers individuals to navigate life’s challenges with greater confidence and control.
DBT is a structured form of psychotherapy that helps individuals manage intense emotions, improve relationships, and develop healthier coping strategies. It blends cognitive behavioral techniques with mindfulness practices and is commonly used to treat borderline personality disorder, depression, anxiety, PTSD, and other emotional regulation challenges.
The four core skills in DBT are mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness. Mindfulness keeps individuals present, distress tolerance helps manage crises, emotion regulation enhances control over feelings, and interpersonal effectiveness improves communication and relationships.
The 24-hour rule means that if a client engages in self-harm or a suicide attempt, the therapist will not offer phone coaching or outside-session support for the next 24 hours. This guideline is designed to avoid reinforcing harmful behaviors with immediate attention and encourages clients to rely on their DBT skills while continuing therapy as scheduled.
CBT focuses on identifying and changing negative thought patterns and behaviors. DBT builds on CBT by adding mindfulness and emotional acceptance, emphasizing a balance between change and self-validation. While CBT helps people think differently, DBT also teaches how to accept reality and respond with practical coping strategies.
DBT may not be suitable for individuals who are unwilling to engage actively in structured sessions or practice skills between meetings. It is also less effective for conditions that do not involve emotional dysregulation, such as specific phobias or thought disorders, where other therapies may be more appropriate.
A typical DBT session includes individual therapy focused on personal goals and skill application, as well as group skills training, where clients learn and practice DBT techniques in a supportive setting. Some programs also offer phone coaching to help clients apply skills during real-life challenges.
At District Behavioral Health Group, we offer comprehensive, evidence-based treatment for individuals seeking support through Dialectical Behavior Therapy (DBT). Our nationwide recovery network ensures a clear, structured care path that guides you every step of the way, combining compassionate support with proven therapies to help you achieve lasting change.
Our comprehensive programming includes:
Individual DBT Therapy: One-on-one sessions focused on building coping strategies, reducing harmful behaviors, and supporting personal goals.
DBT Group Skills Training: Structured group sessions to practice mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness in a supportive setting.
Crisis Coaching & Support: Real-time phone coaching to apply DBT skills during challenging moments.
Partial Hospitalization Programs (PHP): Full-day structured care offering intensive therapy without overnight stays.
Intensive Outpatient Programs (IOP): Flexible part-time programs to balance therapy with daily life responsibilities.
Outpatient Programs (OP): Ongoing support to maintain progress and reinforce DBT skills long-term.
Take the first step toward emotional regulation, healthier relationships, and greater stability. Call our caring team today at (888) 707-6073 to learn more about DBT treatment at District Behavioral Health.
Sources
[2].https://preventionservices.acf.hhs.gov/programs/782/
[3].https://pmc.ncbi.nlm.nih.gov/articles/PMC2963469/
[4].https://www.abct.org/fact-sheets/dialectical-behavior-therapy/
Check out our addiction recovery blog to learn more about substance use disorders and how to get effective treatment.

We strive to provide a comfortable, home-like environment during your recovery journey. Browse our facility images below to take a look at our upscale residential facilities.
Paying Out Of Pocket without Insurance
If you can’t pay your co-pay amount
Paying Out Of Pocket with Insurance
(Depending on insurance plan)
View our wide selection of accepted providers. Don’t see yours? Call our admissions team for help.











Whether you’re seeking help for yourself or a loved one, our admissions team is available 24/7 to answer your questions and guide you toward the right care.

| March | 2026 | |||||
|---|---|---|---|---|---|---|
| March 2026 | ||||||
| SSunday | MMonday | TTuesday | WWednesday | TThursday | FFriday | SSaturday |