Home
Locations 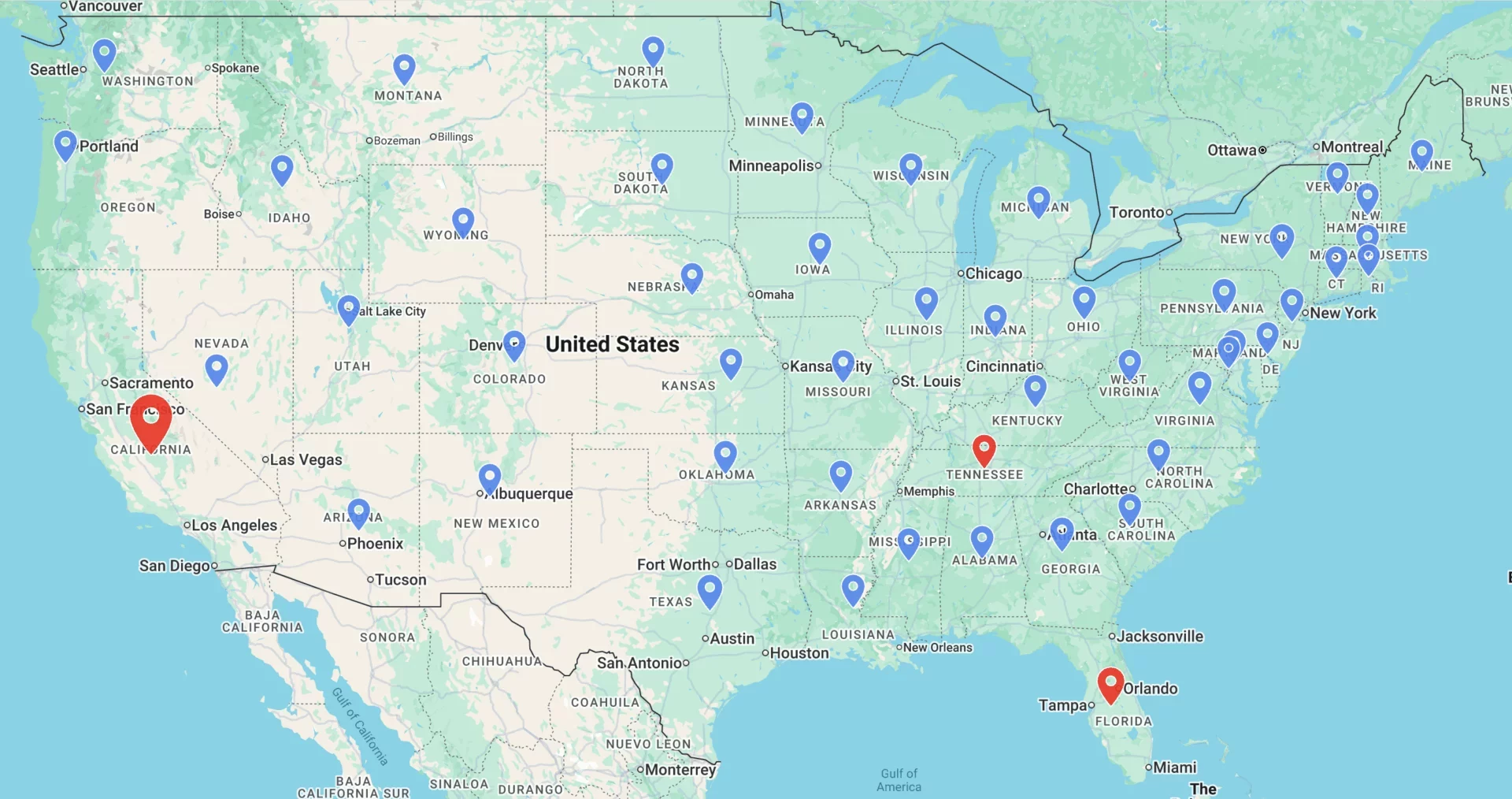
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions

Home
Locations 
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions








Matthew D'Ursov

Amy Leifeste

Karena Mathis



Living with both a mental health condition and substance use can feel overwhelming, especially when symptoms feed into each other. Many people seeking dual diagnosis rehab feel frustrated by past treatment attempts that only addressed one side of the problem. Our dual diagnosis rehab is built for this exact challenge, providing coordinated care that treats mental health and addiction together rather than in isolation. This approach helps people finally understand what is driving their behaviors and how to stabilize both areas at once.
Our programs are delivered through the District Behavioral Health network and supported by specialized care at Renaissance Recovery, offering structured therapy, psychiatric oversight, and ongoing clinical coordination. This level of care works because it targets the full picture, not just surface-level behaviors.
See more about our Dual Diagnosis Rehab program below.
Our behavioral health services support men and women struggling with substance use and co-occurring mental health disorders. District Behavioral Health focuses on providing a comprehensive continuum of care, including personalized outpatient treatment, intensive outpatient (IOP) and partial hospitalization programs (PHP), and coordinated support services designed to help individuals stabilize, develop effective coping skills, and build lasting recovery within their communities.
When mental health and addiction co-occur, it can be particularly complicated to find appropriate care. It poses a dual diagnosis, necessitating a treatment approach that simultaneously tackles both issues. A Dual Diagnosis Treatment facility is structured to deliver that type of care. These holistic approaches integrate mental health therapies with substance use treatment to promote recovery and long-term stability.
If you are searching for “Dual Diagnosis Treatment Centers Near Me,” understanding how these programs work and what to expect can help you or your loved one make the right decision for recovery.
A dual diagnosis means that a person is living with both a mental health disorder and a substance use disorder at the same time [1]. For instance, one may suffer from depression in addition to alcohol use disorder. They may co-occur, complicating the healing process if only one is addressed.
Co-morbidity is the norm, but poses a specific type of treatment that addresses both mental illness and addiction in conjunction. Dual diagnosis programs are essential for lasting healing because, untreated, the symptoms will often worsen.
Several mental health conditions are frequently associated with substance use disorders. Depression, anxiety disorders, bipolar disorder, and post-traumatic stress disorder (PTSD) are among the most common. Some may self-medicate through drug or alcohol use, which only exacerbates both conditions in the long run. The diagnostic co-morbidity between addiction and these mental health conditions underscores an argument for co-treatment.
The following are some of the more prevalent co-occurring disorders:
Depression: persistent sadness, low energy, and loss of interest.
Anxiety disorders: constant worry, panic attacks, or social anxiety.
Bipolar disorder: extreme mood swings that affect daily life.
Post-traumatic stress disorder (PTSD): distressing flashbacks and emotional triggers.
Personality disorders: unstable emotions and difficulty maintaining relationships.
Dual diagnosis requires specialized treatment because both conditions, that is, mental health disorders and substance use disorders, interact and influence each other [2]. If only one is treated, the other usually remains untreated and may soon result in relapse or exacerbation of symptoms.
There are specialized sets of programming created to treat both conditions concurrently in such a manner that therapy, medication management, and support all work together as one united process. Such care leads to better recovery, fewer complications, and helps patients find long-term recovery.
Co-occurring disorders can be hard to recognize because symptoms of mental illness and substance use often overlap. Individuals involved might experience behavioral, affective, or physical health symptoms that appear to connect the two.
These signs of “trouble” include anything from emotional distress to difficulties at work, school, or in a personal relationship. Co-occurring mental health symptoms and addiction often exacerbate each other. Recognizing the symptoms early on can lead to appropriate care and prevent disease progression.
Common signs and symptoms include:
Mood changes such as sadness, irritability, or sudden anger.
Increased substance use to cope with stress or emotions.
Withdrawal from family and friends can lead to isolation.
Difficulty managing daily responsibilities, such as work or studies.
Sleep problems such as insomnia or oversleeping.
Worsening mental health symptoms when substance use increases.
An individual who has both a mental health disorder and a substance use disorder will exhibit observable behavioral differences. These changes may begin mild and progress to more significant ones as each condition advances. These changes are usually first detected by family, friends, or coworkers. But these behavior changes are identified early on to help seek assistance and prevent the condition from escalating.
Some common behavioral changes include:
Emotional problems were frequently identified as a robust predictor of an individual having both a mental health condition and a substance use disorder. These are signs that can disrupt relationships, work performance, and well-being. When feeling emotional, oftentimes people seek out drugs or alcohol as a coping mechanism, which then exacerbates the issue. Being cognizant of the emotional warning signs can play a pivotal role in early diagnosis and intervention.
Some warning labels in the emotional arena are:
Feelings of sadness or hopelessness that remain over time.
Rapid cycling between high and low moods.
Generalized anxiety or fear for no apparent reason.
Guilt or feelings of worthlessness that are disruptive to everyday life.
Marked irritability or frustration over small matters.
Inability to cope with stressful situations, resulting in emotional outbursts.
There is no singular reason for the occurrence of co-occurring disorders. Rather, they tend to arise from a combination of genetic, biological, and environmental influences. Having a family history of mental illness or addiction is one risk factor, while experiencing a traumatic life event, ongoing stress, or using drugs at an early age can heighten the risk even further.
Substance use or abuse frequently begins in the context of untreated mental health symptoms, resulting in addiction. Alternatively, substance use can also be a direct cause or exacerbation of mental health disorders. Conditions such as these contribute to the complexity of dual diagnosis and the need for treatment that concurrently addresses both conditions.
The co-occurrence of disorders is significantly influenced by genetics and biology. Those with a family history of mental illness or substance use conditions are at higher risk for both. Also, imbalances in the brain’s chemistry and adaptations in the brain’s reactions to stress represent biological elements behind these disorders [4].
These are not necessarily predictors for the likelihood of a dual diagnosis, but are risk factors that enhance susceptibility, particularly in conjunction with environmental precipitating factors.
Key genetic and biological risk factors include:
A family history of either addiction or mental illness, increasing vulnerability.
Chemistry imbalances in the brain are related to mood, stress, and decision-making.
Genetic predispositions that render individuals more sensitive to drugs or alcohol.
An altered emotional appraising chronic stress response.
Substance exposure at a young age interferes with typical brain development.
Chronic stress and consistent life challenges are major risk factors for co-occurring disorders. Chronic stress leads to deterioration of mental health and drives one to maladaptive coping mechanisms like the use of alcohol or drugs. These behaviors can eventually lead to addiction, compounding existing mental health concerns.
Difficulties such as money issues, unstable relationships, or work stress can also create obstacles to recovery. Treating stress is also relevant in dual diagnosis because it lessens triggers for relapse.
Common stress-related risk factors include:
Financial problems are a constant source of worry.
Relationships that are unstable or toxic cause emotional strain.
Workplace stress/pressure resulting in burnout/unhealthy coping.
Chronic caregiving is emotionally depleting.
Chronic health problems that heighten emotional and physical stress.
Treatment for co-occurring disorders is offered at different levels, depending on how severe the mental health and substance use issues are. Some people may benefit from outpatient care, where they attend therapy sessions while continuing with daily life. Others may need more structured programs, such as inpatient or residential treatment, where 24-hour support is provided.
Coordination of outpatient treatment is intended for those with a less severe co-occurring disorder. Patients can continue to work or attend school and reside at home while receiving therapy or counseling. This is more concerned with skills, triggers, coping, and functioning. Patients who have good support systems and are highly motivated do best in outpatient programs.
Institutional settings, such as inpatient and residential programs, are appropriate for individuals with severe co-occurring conditions who require more structured, 24-hour intensive programs. In these programs, mental health and substance use are treated simultaneously in a safe and supportive environment.
They provide treatment, medical care, and around-the-clock support for patients who live on-site. Some even argue that this sufficient level of treatment stabilizes symptoms and significantly reduces the risk of relapse, strengthening the foundation on which recovery will be built.
Key features of inpatient and residential programs include:
24/7 medical supervision to monitor health and safety.
Individual and group therapy to address both conditions.
Medication management for mental health and addiction.
Structured daily routines that encourage stability and healthy habits.
Supportive environment away from triggers and negative influences.
Care doesn’t stop when a program is over; Aftercare is crucial in caring for co-occurring disorders. This can be important to sustain progress, cope with stress, and avoid relapse. Aftercare may take the form of continued therapy, support groups for peers, appointments for check-ins with a mental health expert, etc. Such services offer a support and accountability system when re-entering the real world. Effective aftercare equips a person to face obstacles and work towards a healthy future.
Outpatient therapy for continued emotional and behavioral support.
12-step or peer recovery groups for shared experiences and motivation.
Medication management to stabilize mental health symptoms.
Sober living homes provide structured, substance-free environments.
Life skills training to improve independence and daily functioning.
A correct diagnosis of co-occurring disorders can be difficult because the symptoms of mental illness and substance use frequently overlap. A complete assessment of these diagnoses is also important to understand both conditions and design an adequate treatment. Practitioners in medicine and mental health generally start with an exhaustive medical history that covers family history, history of substance use, and psychiatric symptoms.
Both disorders are screened for using standardized screening tools as well as psychological assessments. Occasionally, lab tests will be done to assess general health and the impact of use. An accurate diagnosis means getting simultaneous treatment for mental illness and addiction, which is required for recovery in the long term.
Effective management and treatment of co-occurring disorders requires a comprehensive approach that addresses both mental health conditions and substance use simultaneously. Plans are tailored to the individual and consist of therapy, medication, and lifestyle support for recovery.
Psychotherapy, such as cognitive-behavioral therapy and dialectical behavior therapy, helps patients identify and modify dysfunctional thoughts and behaviors. Pharmaceuticals can be used to address the symptoms of mental illness, decrease cravings, or assist with detox.
Dual diagnosis treatment involves the co-occurring treatment of mental disorders as well as those related to substance abuse through therapeutic experience, pharmaceutical support, and counseling to improve rates of recovery as well as relapse.
What Are the Barriers to Dual Diagnosis Treatment?
Barriers include lack of awareness, stigma, limited access to integrated care, inadequate insurance coverage, and fragmented treatment systems, which often treat mental health and addiction separately rather than together.
Risks include worsening mental health symptoms, increased substance dependence, higher likelihood of relapse, strained relationships, impaired functioning at work or school, and greater difficulty achieving long-term recovery without integrated care.
The modern term often used is “co-occurring disorders,” which emphasizes the simultaneous presence of both a mental health disorder and a substance use disorder, reflecting a more integrated treatment approach.
One such example is an individual with major depressive disorder comorbid with alcohol use disorder. Depression can cause drinking, and alcohol use can exacerbate depressive symptoms, creating a cycle that requires integrated care.
Benefits include improved symptom management, reduced relapse risk, enhanced overall well-being, better coping strategies, coordinated care, stronger support systems, and higher chances of achieving long-term recovery and stability.
At District Behavioral Health Group, we provide comprehensive, evidence-based care for individuals living with both mental health disorders and substance use disorders. Our nationwide network ensures a seamless, connected journey that supports recovery every step of the way.
Our specialized dual diagnosis programming includes:
Medication-Assisted Detox: Medically supervised detox with FDA-approved medications to manage withdrawal safely.
Crisis Intervention & Stabilization: Immediate mental health support to restore safety and stability.
Inpatient & Residential Programs: 24/7 live-in care combining therapy, medical support, and structured routines.
Partial Hospitalization Programs (PHP): Intensive daily treatment without overnight stays for structured recovery.
Intensive Outpatient Programs (IOP): Flexible part-time therapy to balance treatment with daily life.
Outpatient Programs (OP): Ongoing sessions to maintain progress and support long-term stability.
To explore our dual diagnosis recovery programs, call our dedicated team today at (888) 707-6073.
Sources:
[1] https://medlineplus.gov/dualdiagnosis.html
[2] https://effectivehealthcare.ahrq.gov/health-topics/dual-diagnosis
[3] https://docs.google.com/document/d/1i16pjCUJq_LG7_iQ-NrjUXZzlvXejR2RTMMUKetKmJg/edit?tab=t.0#heading=h.ypqq4m1ctnb0
[4] https://www.nimh.nih.gov/health/topics/substance-use-and-mental-health
Check out our addiction recovery blog to learn more about substance use disorders and how to get effective treatment.

We strive to provide a comfortable, home-like environment during your recovery journey. Browse our facility images below to take a look at our upscale residential facilities.
Paying Out Of Pocket without Insurance
If you can’t pay your co-pay amount
Paying Out Of Pocket with Insurance
(Depending on insurance plan)
View our wide selection of accepted providers. Don’t see yours? Call our admissions team for help.











Whether you’re seeking help for yourself or a loved one, our admissions team is available 24/7 to answer your questions and guide you toward the right care.

| March | 2026 | |||||
|---|---|---|---|---|---|---|
| March 2026 | ||||||
| SSunday | MMonday | TTuesday | WWednesday | TThursday | FFriday | SSaturday |