Home
Locations 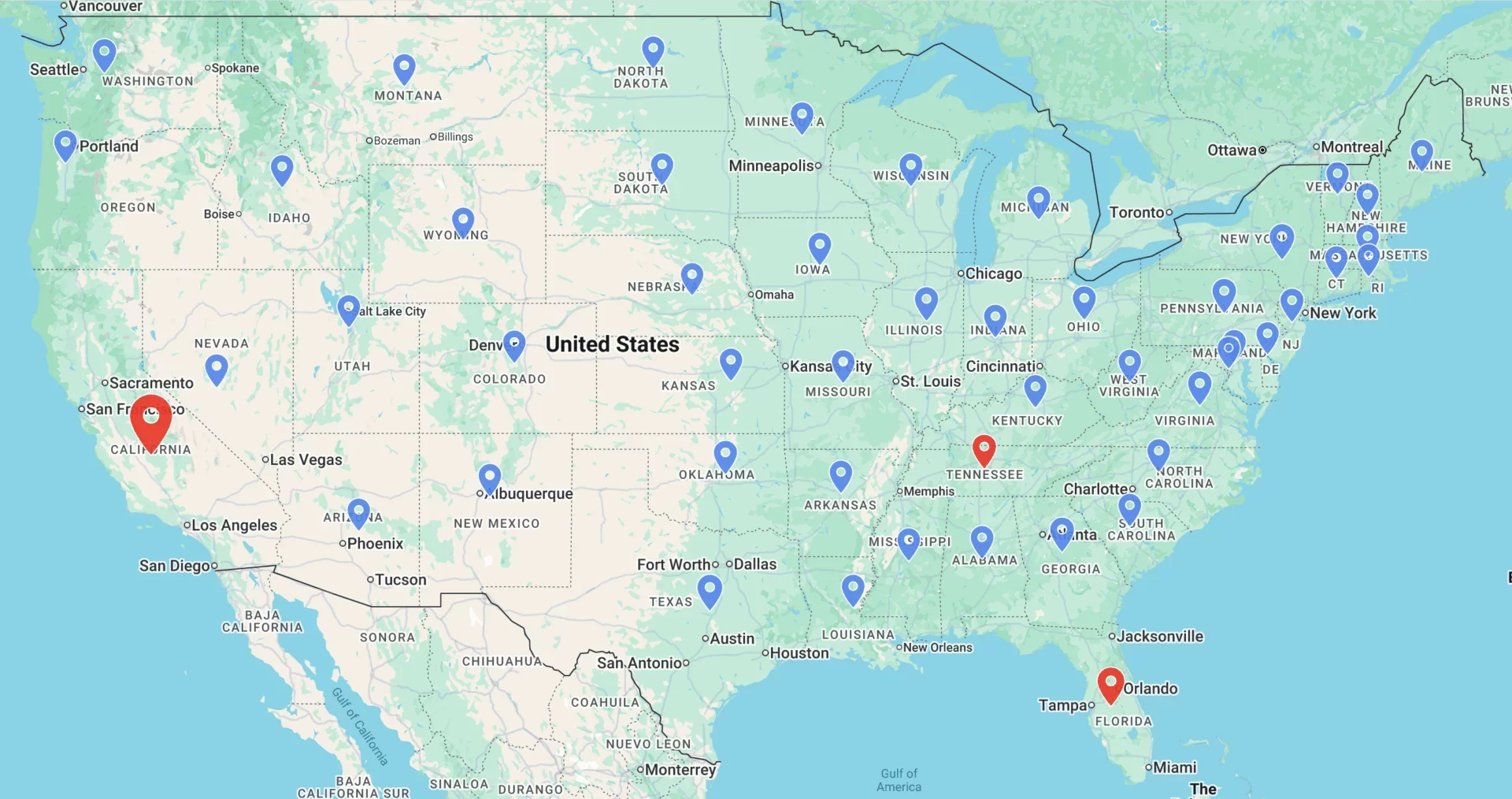
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions

Home
Locations 
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions








Matthew D'Ursov

Amy Leifeste

Karena Mathis



Living with addiction can quietly disrupt health, focus, and emotional balance, even when life on the surface appears stable. Many people hesitate to seek treatment because stepping away from work or family does not feel realistic. MAT Therapy is created for individuals at this stage, offering medically guided care that supports recovery while allowing daily life to continue. It provides structure without forcing distance from the responsibilities that cannot be paused.
District Behavioral Health offers MAT Therapy through the Renaissance Recovery network. These outpatient programs combine medication support, behavioral therapy, and practical recovery planning without requiring overnight stays. This approach helps individuals regain stability, improve functioning, and build long-term recovery while remaining active in everyday life.
See more about our MAT Therapy program below.
Our behavioral health services support men and women struggling with substance use and co-occurring mental health disorders. District Behavioral Health focuses on providing a comprehensive continuum of care, including personalized outpatient treatment, intensive outpatient (IOP) and partial hospitalization programs (PHP), and coordinated support services designed to help individuals stabilize, develop effective coping skills, and build lasting recovery within their communities.
Struggling with alcohol or drug use can affect every aspect of a person’s life, from their health to their relationships and work. Finding the right treatment can feel overwhelming, especially with so many options available. One approach that has helped countless people regain control is Medication-Assisted Treatment (MAT).
MAT blends FDA-approved medications with counseling and behavioral therapies to make recovery safer and more sustainable. If you’ve been searching for “medication-assisted treatment for substance use disorder near me,” this guide will explain how it works, what medications are used, and what you can expect on your journey to recovery.
Medication-Assisted Treatment (MAT) is an evidence-based approach that combines prescription medications with counseling and support services to treat substance use disorders [1]. While traditional methods often focus solely on therapy, MAT uses approved medications to manage withdrawal symptoms and reduce cravings, making it easier for individuals to focus on their recovery.
MAT is not about replacing one drug with another; it’s about using specific, controlled medications to stabilize the brain and body, creating a solid foundation for healing. This “whole-patient” approach is recognized and supported by leading healthcare organizations across the United States as a gold standard of care. It has been proven to improve patient survival, increase treatment adherence, and reduce the risk of relapse.
MAT provides comprehensive care for individuals with substance use disorders. Its primary goals are to reduce cravings, prevent relapse, and support long-term recovery. By combining medication with therapy, MAT addresses both the biological changes caused by addiction and the emotional challenges that accompany it.
Medications used in MAT help restore normal brain function, reduce withdrawal symptoms, and curb cravings. Therapy complements this by teaching coping strategies, addressing underlying emotional issues, and building resilience. Together, they form an integrated treatment plan that supports both physical stability and emotional well-being.
MAT is supported by decades of research and clinical practice. Studies consistently show that it reduces the risk of relapse, improves treatment retention, and enhances long-term recovery outcomes. It is considered one of the safest and most effective treatments for opioid and alcohol use disorders when provided under medical supervision.
A common myth is that MAT simply substitutes one drug for another. In reality, the medications used—such as buprenorphine, methadone, and naltrexone—are carefully regulated, clinically approved, and designed to support recovery without creating new addictions. Misunderstandings about MAT can discourage people from seeking help, making education and awareness essential.
MAT offers multiple benefits beyond managing cravings. It can improve mental clarity, reduce the risk of relapse, and help individuals regain stability in daily life. For many, MAT serves as a pathway to long-term health, independence, and a more hopeful future.
MAT is a comprehensive approach that encompasses several key components working in tandem [2]. Treatment is always tailored to fit each person’s unique needs.
FDA-Approved Medications: Medications are the cornerstone of MAT. They are rigorously tested and approved by the Food and Drug Administration (FDA) to target the brain functions involved in addiction, which helps alleviate withdrawal symptoms and reduce cravings.
Behavioral Therapies: Therapy is just as crucial as medication. Behavioral therapies, such as Cognitive Behavioral Therapy (CBT), help patients identify the root causes of their addiction, develop healthy coping skills, and learn to manage stress and emotional triggers.
Counseling and Support Programs: Group sessions, individual counseling, and peer support groups provide emotional guidance and a sense of community. These resources create a network of accountability and understanding, making the recovery journey feel less isolating.
Ongoing Medical Supervision: Regular medical supervision ensures that the treatment is both safe and effective. A doctor monitors the patient’s progress, adjusts medication dosages as needed, and manages any side effects, building a foundation of trust and support.
For alcohol use disorder, one of the most common substance use disorders, MAT offers several effective medications. These medications work by either reducing cravings or creating a negative physical reaction to alcohol. When combined with therapy, they provide powerful tools for preventing relapse.
Naltrexone: This medication works by blocking the euphoric and rewarding effects of alcohol in the brain. When the enjoyable sensation is removed, the motivation to drink often decreases significantly.
Acamprosate: Best for individuals who have already stopped drinking, acamprosate helps restore the natural chemical balance in the brain that was disrupted by long-term alcohol use. This can ease withdrawal symptoms and reduce cravings.
Disulfiram: This medication works differently by creating a strong physical deterrent to drinking. If a person taking disulfiram consumes alcohol, they will experience unpleasant side effects like nausea and flushing.
Naltrexone: Headache, nausea, fatigue (usually temporary).
Acamprosate: Diarrhea, mild anxiety, or sleep changes.
Disulfiram: No issues if alcohol is avoided; reactions occur only with alcohol use.
Safety checks: Doctors screen for potential drug interactions and closely monitor patients’ health to minimize risks.
Before prescribing, healthcare providers assess:
Medical history and co-existing conditions.
Addiction patterns and readiness for change.
Treatment goals.
Follow-up visits ensure the medication is effective, safe, and well-tolerated.
Safety: These medications are safe for long-term use under medical supervision.
Monitoring: Regular lab tests check for rare complications, such as liver strain.
Duration: Many patients remain on MAT for months or years, tapering only when stable.
Outcome: For most, the benefits—sustained sobriety, improved health, and stability—far outweigh the risks.
Opioid use disorder is a complex condition that often requires a specialized approach. MAT offers several medications that effectively reduce cravings and withdrawal symptoms, allowing individuals to stabilize their lives and focus on recovery.
Methadone: Used for decades, methadone is a full opioid agonist that relieves withdrawal symptoms and cravings. When taken as prescribed, it does not produce a “high” but allows for stabilization, often requiring daily visits to a specialized clinic.
Buprenorphine: A partial opioid agonist, buprenorphine reduces cravings and withdrawal without producing the intense effects of full opioids like heroin. It has a lower risk of misuse and can often be prescribed in an office-based setting, offering more flexibility.
Naltrexone: As an opioid antagonist, naltrexone completely blocks the effects of opioids. It is not an opioid itself and has no potential for misuse. It is best suited for individuals who have already completed detoxification.
A medical professional will help determine the best option based on a patient’s needs, medical history, and treatment goals.
|
Medication |
How It Works |
Access & Use |
Key Considerations |
|
Methadone |
Full agonist; prevents withdrawal and cravings |
Daily clinic visits |
Highly effective but requires a structured setting |
|
Buprenorphine |
Partial agonist; reduces cravings with lower misuse risk |
Office-based prescription |
More flexible, widely used in outpatient care |
|
Naltrexone |
Antagonist: blocks opioid effects |
Daily pill or monthly injection (after detox) |
No opioid-like effects; requires full detox first |
Supervision is essential: All opioid MAT medications must be prescribed and monitored by a healthcare professional.
Possible side effects: May include nausea, constipation, sleep changes, or mild mood effects, depending on the medication.
Safety checks: Doctors adjust doses, monitor progress, and screen for interactions to ensure treatment remains safe and effective.
Ongoing care: Regular follow-ups help patients stay engaged and supported throughout recovery.
Yes. Most insurance plans, including Medicaid and Medicare, cover Medication-Assisted Treatment (MAT) as an essential behavioral health service. Federal laws require parity, meaning addiction treatment must be covered on the same level as other medical conditions. While private insurance policies vary, many include both medications and therapy. Verifying coverage early helps avoid unexpected costs and ensures a smoother start to treatment.
Mental Health Parity and Addiction Equity Act (MHPAEA): Requires insurers to cover substance use treatment, including MAT, on equal terms with other medical care [3].
Affordable Care Act (ACA): Expanded access through insurance marketplaces and mandated coverage for substance use disorder services [3].
State protections: Many states add their own requirements, further strengthening access to evidence-based addiction care.
Most private insurers cover MAT medications (e.g., buprenorphine) and counseling.
Pre-authorization may be required before starting treatment.
Coverage often depends on in-network providers.
If coverage is denied, patients can file an appeal based on medical necessity.
Many plans now cap copays for behavioral health services, making care more affordable.
Medicaid: Covers MAT in all states, including methadone provided in certified clinics.
Medicare Part B: Covers outpatient therapy and MAT medications after the deductible.
Both programs prioritize access for low-income individuals and older adults.
ACA expansions increased enrollment, ensuring more people are eligible for coverage.
Copays: Typically $10–$50 per session or prescription.
Deductibles: May reach $1,000 or more annually, depending on the plan.
Residential treatment: May involve higher costs if not fully covered.
Uninsured patients: Sliding-scale clinics and state-funded programs can help.
Call your insurer’s member services line and ask about MAT coverage.
Provide procedure codes (e.g., H00031 for therapy) for accurate information.
Ask about medication limits, referrals, or prior authorization requirements.
Many treatment centers will verify benefits on your behalf.
Online insurance portals can show real-time coverage details.
The duration of MAT varies for each patient. Some may use medication for a few months to navigate early recovery, while others may benefit from it for several years or even for life. There is no one-size-fits-all timeline. The focus is on finding a duration that supports stable, long-term recovery.
Factors that influence treatment length include:
The type of substance used and the severity of the addiction.
The patient’s overall physical and mental health.
The individual’s response to medication and therapy.
The strength of their support system.
When it is time to transition off medication, a doctor will create a gradual tapering plan to ensure the process is safe and comfortable.
Medication-Assisted Treatment (MAT) is an approach that combines FDA-approved medications with counseling and behavioral therapies to treat substance use disorders. It helps reduce cravings and manage withdrawal, supporting long-term recovery.
For opioid use disorder, common drugs are methadone, buprenorphine, and naltrexone. For alcohol use disorder, they include naltrexone, disulfiram, and acamprosate.
No. Methadone is just one of several medications that can be used within a MAT program. MAT is a comprehensive treatment approach that also includes therapy, counseling, and other support services.
While this varies by individual, opioids like heroin and fentanyl are often considered among the most difficult to quit due to the severity of withdrawal symptoms, intense cravings, and high relapse rates.
Like any medical treatment, MAT has risks, such as medication side effects or the potential for medication misuse. However, when managed by a trained medical professional, the proven benefits of MAT—including preventing overdose and supporting recovery—far outweigh the risks.
Not exactly. “Rehab” is a broad term for various recovery programs. MAT is a specific treatment modality that can be a core component of a comprehensive rehab program, whether in an inpatient or outpatient setting.
At District Behavioral Health Group, we provide evidence-based care for individuals struggling with substance use disorder and co-occurring mental health challenges. Our nationwide recovery network ensures a clear, connected treatment path, offering support at every stage of recovery. From detox to long-term outpatient care, our programs are designed to restore health, stability, and independence.
Our comprehensive programming includes:
Medication-Assisted Detox: Safe, medically supervised detox to manage withdrawal symptoms.
Crisis Intervention & Stabilization: Immediate care to ensure safety during moments of crisis.
Inpatient & Residential Programs: 24/7 structured treatment with therapy, medical support, and daily routines in a healing environment.
Partial Hospitalization Programs (PHP): Intensive daytime therapy without overnight stays.
Intensive Outpatient Programs (IOP): Flexible part-time treatment balancing therapy with daily life.
Outpatient Programs (OP): Continued therapy to maintain recovery while living independently.
If you or someone you love is struggling with substance use disorder, call our caring team today at (888) 707-6073 and begin the path toward recovery.
[1] https://www.fda.gov/drugs/information-drug-class/information-about-medications-opioid-use-disorder-moud
[2] https://pmc.ncbi.nlm.nih.gov/articles/PMC7278292/
[3] https://www.cms.gov/marketplace/private-health-insurance/mental-health-parity-addiction-equity
Check out our addiction recovery blog to learn more about substance use disorders and how to get effective treatment.

We strive to provide a comfortable, home-like environment during your recovery journey. Browse our facility images below to take a look at our upscale residential facilities.
Paying Out Of Pocket without Insurance
If you can’t pay your co-pay amount
Paying Out Of Pocket with Insurance
(Depending on insurance plan)
View our wide selection of accepted providers. Don’t see yours? Call our admissions team for help.











Whether you’re seeking help for yourself or a loved one, our admissions team is available 24/7 to answer your questions and guide you toward the right care.

| March | 2026 | |||||
|---|---|---|---|---|---|---|
| March 2026 | ||||||
| SSunday | MMonday | TTuesday | WWednesday | TThursday | FFriday | SSaturday |