Home
Locations 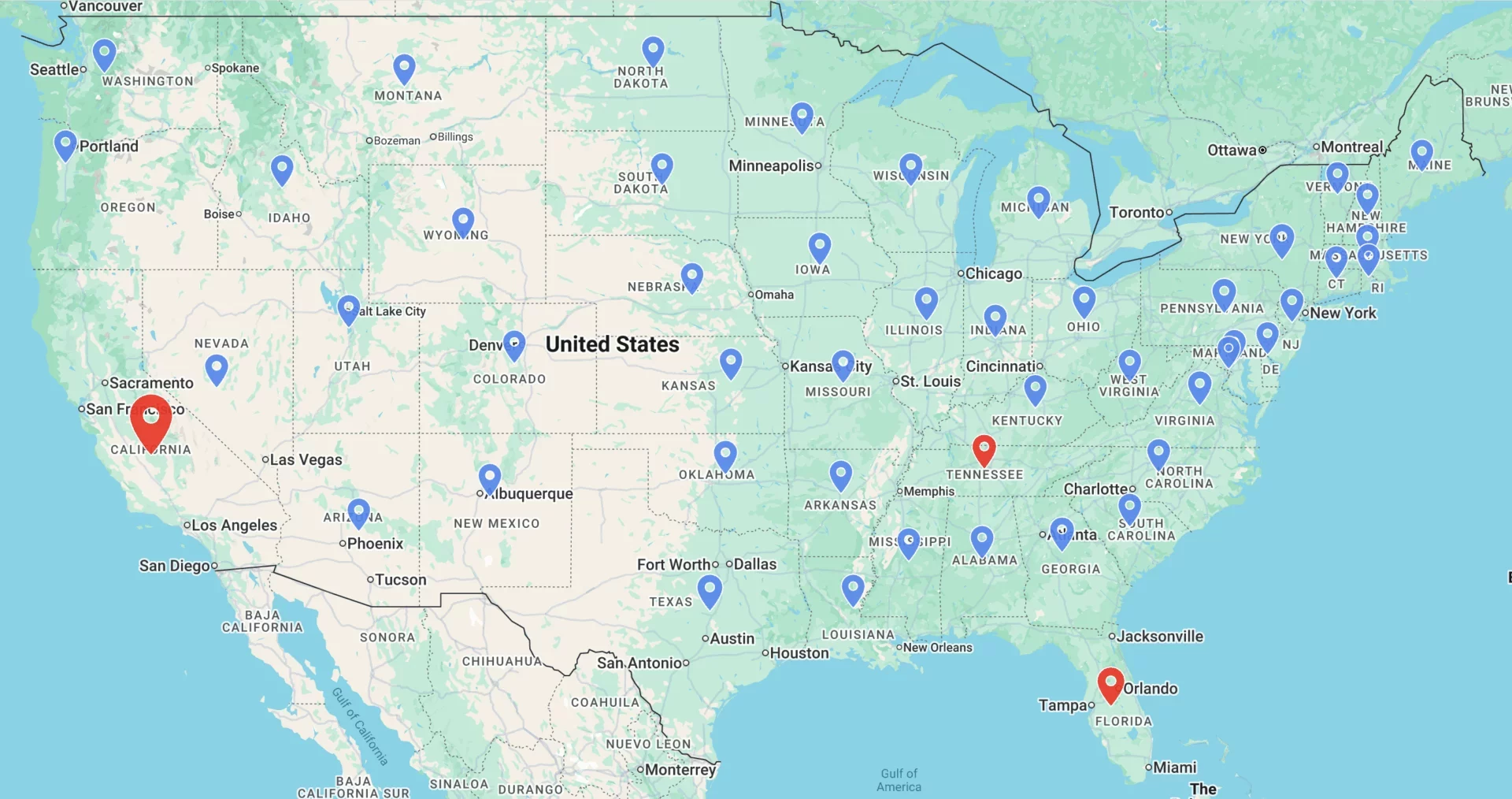
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions

Home
Locations 
Locations

Treatments Programs 
Treatments Programs

Drug Addictions 
Contact UsDrug Addictions








Matthew D'Ursov

Amy Leifeste

Karena Mathis



Xanax use often begins as a way to manage anxiety, panic, or stress, but over time it can quietly take control of daily functioning. Tolerance can develop quickly, leading to increased doses just to feel normal. When attempts to stop cause rebound anxiety, insomnia, or physical discomfort, many people feel stuck between dependence and fear of withdrawal. This uncertainty makes it difficult to know when rehab is needed or what type of treatment is safest.
• Xanax use can escalate quickly due to tolerance
• Dependence may form even with prescribed use
• Withdrawal symptoms increase fear of stopping
• Structured rehab supports safe stabilization
Renaissance Recovery offers Xanax Rehab through the District Behavioral Health network, providing structured outpatient care focused on gradual tapering, emotional regulation, and long-term stability. For individuals whose Xanax use is closely tied to anxiety, trauma, or mood disorders rather than addiction alone, Xanax-related mental health treatment is also available through Connections Mental Health, part of the DBH family of care. These programs work together to match treatment to individual needs.
Xanax rehab helps restore balance and confidence. See more about our Xanax rehab program below.
Our behavioral health services support men and women struggling with substance use and co-occurring mental health disorders. District Behavioral Health focuses on providing a comprehensive continuum of care, including personalized outpatient treatment, intensive outpatient (IOP) and partial hospitalization programs (PHP), and coordinated support services designed to help individuals stabilize, develop effective coping skills, and build lasting recovery within their communities.
Xanax, with the generic name alprazolam, is one of the most widely prescribed medications for managing anxiety and panic disorders. As a fast-acting benzodiazepine, it can provide immediate relief from debilitating symptoms. However, its effectiveness is matched by a high potential for misuse, dependence, and addiction. When Xanax use spirals out of control, it can have devastating consequences on a person’s health, relationships, and overall quality of life.
At District Behavioral Health, we provide comprehensive and compassionate addiction treatment to help individuals safely navigate withdrawal, address the root causes of their addiction, and build a strong foundation for long-term recovery.
This article discusses Xanax addiction’s nature, signs and symptoms, treatment options, potential dangers, key statistics, and strategies for effective treatment and relapse prevention.
Xanax addiction occurs when a person develops physical or psychological dependence on the drug, often after long-term or excessive use. This dependence can happen even with prescribed use if taken longer than recommended. Xanax belongs to the benzodiazepine class of medications, which act on the brain and central nervous system to produce a calming effect [1].
While Xanax can be a lifeline for individuals with severe anxiety or panic disorders, its mechanism of action also makes it highly susceptible to misuse. Even when taken as prescribed, regular use can lead to tolerance, a state where the body requires increasingly higher doses to achieve the initial desired effect. This escalating use often creates a dangerous cycle that can quickly spiral into addiction.
Key Aspects of Xanax Addiction
Physical Dependence: This occurs when the body adapts to the presence of Xanax and experiences withdrawal symptoms if the medication is stopped or the dosage is reduced. Symptoms can range from uncomfortable to life-threatening.
Psychological Dependence: This involves a perceived need to use Xanax to cope with daily life, manage emotions, or feel “normal.” The person may feel intense anxiety or panic at the thought of not having the drug.
Co-Occurring Disorders: Xanax addiction often exists alongside other mental health conditions, such as depression, generalized anxiety disorder, or post-traumatic stress disorder (PTSD). This is known as a dual diagnosis and requires integrated treatment.
Recognizing the signs of a Xanax addiction can be challenging, as they often develop gradually. The symptoms can be categorized into physical, psychological, and behavioral changes.
Physical Symptoms
Persistent Drowsiness and Fatigue: Appearing constantly tired, lethargic, or sedated.
Slurred Speech and Poor Coordination: Difficulty speaking clearly and a lack of balance, similar to being intoxicated.
Cognitive Impairment: Noticeable memory problems, confusion, and difficulty concentrating.
Changes in Appearance: A general lack of attention to personal hygiene or grooming.
Physical Withdrawal Symptoms: Experiencing tremors, sweating, headaches, muscle pain, and insomnia when not using the drug.
Psychological Symptoms
Intense Cravings: An overwhelming and persistent urge to use Xanax.
Anxiety and Rebound Panic: Experiencing a worsening of anxiety symptoms when the effects of the drug wear off.
Mood Swings: Unexplained shifts between irritability, depression, and periods of euphoria.
Emotional Blunting: A reduced ability to feel pleasure or other emotions.
Behavioral Symptoms
Increased Dosage: Taking more Xanax than prescribed or using it more frequently.
“Doctor Shopping”: Visiting multiple doctors to obtain several prescriptions.
Secretive Behavior: Hiding the amount of Xanax being used or lying about it.
Social Withdrawal: Isolating from family and friends to hide the addiction or to use the drug.
Neglecting Responsibilities: Failing to meet obligations at work, school, or home due to drug use.
Financial Problems: Spending a significant amount of money to obtain the drug, potentially leading to debt or theft.
How do people abuse xanax?
Standard methods include crushing pills for snorting or combining with alcohol, which heightens risks.
If you’re wondering if one .25 xanax a day is addictive, even low doses can lead to dependence over time. Early recognition of these signs is crucial for seeking xanax addiction treatment centers.
Effective Xanax addiction treatment requires a comprehensive and individualized approach. Because abrupt cessation can be dangerous, treatment must begin with a medically supervised detoxification process, followed by intensive therapy and long-term support [2].
Medical Detox and Tapering
The first and most critical step is a safe, medically supervised detox. Stopping Xanax “cold turkey” can trigger severe withdrawal symptoms, including seizures, hallucinations, and delirium. To prevent this, a gradual tapering schedule is implemented.
The Tapering Process: Under medical supervision, the dosage of Xanax is slowly and systematically reduced over a period of weeks or months.
Medication Support: In some cases, a doctor may switch the person to a longer-acting benzodiazepine, like diazepam (Valium), which is easier to taper. Other medications may be prescribed to manage specific withdrawal symptoms, such as anxiety, insomnia, or nausea.
Individual and Group Therapy
Once the person is physically stable, the psychological aspects of addiction are addressed through therapy.
Cognitive-Behavioral Therapy (CBT): This therapy helps individuals identify and change the negative thought patterns and behaviors that contribute to their addiction.
Dialectical Behavior Therapy (DBT): DBT teaches skills for managing intense emotions, coping with stress, and improving relationships.
Group Therapy: Sharing experiences with peers in a supportive group setting can reduce feelings of shame and isolation.
Relapse Prevention Planning
A core component of treatment is developing a robust relapse prevention plan. This involves learning to identify personal triggers for Xanax cravings and developing healthy coping strategies to manage them.
Xanax is FDA-approved for the treatment of generalized anxiety disorder (GAD) and panic disorder. Its fast-acting nature makes it effective for providing immediate relief from acute symptoms [3].
However, this rapid onset is also what makes it prone to misuse and dependence, especially when taken for extended periods or outside of strict medical guidelines. Doctors typically limit prescriptions to 2-4 weeks to avoid dependence.
Xanax is often prescribed in the context of mental health treatment, but its misuse can paradoxically worsen psychiatric conditions. While it may offer temporary relief from anxiety, long-term dependence can lead to depression, mood instability, and increased emotional dysregulation [4].
Many individuals struggling with Xanax addiction also have a co-occurring mental health disorder, such as:
Depression
Post-traumatic stress disorder (PTSD)
Bipolar disorder
Other substance use disorders (e.g., alcohol or opioids)
Effective Xanax addiction treatment must address both the addiction and the underlying mental health condition simultaneously. This integrated, dual-diagnosis approach is essential for achieving lasting recovery.
Prolonged use of Xanax carries significant health risks that affect cognitive function, physical health, and overall safety.
Dangers of prolonged xanax use include:
Cognitive Decline: Long-term use can lead to persistent memory impairment, difficulty concentrating, and a decline in problem-solving abilities.
Physical Dependence and Severe Withdrawal: The body can quickly become dependent on Xanax, making it incredibly difficult to stop without experiencing a painful and potentially dangerous withdrawal syndrome.
Increased Risk of Accidents: The sedative effects of Xanax, such as drowsiness and poor coordination, significantly increase the risk of falls, car accidents, and other injuries.
Worsening Mental Health: Chronic use can exacerbate underlying conditions like depression and may even lead to an increase in suicidal thoughts.
Risk of Overdose: The risk of a fatal overdose is dramatically amplified when Xanax is mixed with other central nervous system depressants, such as alcohol or opioids. This combination can cause severe respiratory depression, leading to stopped breathing.
Xanax addiction statistics reveal the widespread impact of this drug:
Over 16 million prescriptions for alprazolam were dispensed in the U.S. in 2023, making it one of the most prescribed benzodiazepines [5].
Approximately 4.8 million adults misused benzodiazepines like xanax in 2023, with misuse accounting for about 17% of overall use [6].
Studies indicate that 1 in 3 people using benzodiazepines for more than four weeks develop dependence [7].
Benzodiazepine-related emergency department visits reached over 200,000 in 2023, often involving xanax combined with other substances [8].
Xanax is among the top misused prescription drugs for young adults aged 18-25, with rates higher than in previous years [9].
In 2024 surveys, 2.2% of adults reported benzodiazepine misuse, with xanax leading the category [10].
These statistics highlight why early recognition and treatment of Xanax dependence are critical. Data from the National Survey on Drug Use and Health shows that misuse is declining slightly but remains a public health concern, emphasizing the need for accessible xanax addiction treatment [11].
Effective treatment for Xanax addiction extends beyond detoxification; it requires ongoing support for lasting recovery. After a medically supervised taper off Xanax, individuals benefit from therapy, lifestyle changes, and strong community support to reduce relapse risk.
Relapse prevention strategies for Xanax addiction include:
Identifying and Managing Triggers: Learning to recognize the people, places, and emotions that trigger cravings for Xanax.
Developing Healthy Coping Skills: Utilizing techniques such as mindfulness, exercise, journaling, and meditation to effectively manage stress and anxiety.
Building a Strong Support Network: Connecting with sober peers, supportive family members, and clinicians.
Continuing Therapy: Ongoing individual or group therapy to address underlying mental health issues and reinforce coping skills.
At District Behavioral Health, we incorporate relapse prevention into every treatment plan to support individuals in maintaining long-term recovery. Research shows that integrating therapy with ongoing support can cut relapse rates by up to 50% in cases of benzodiazepine addiction [12]. Regular follow-ups and comprehensive aftercare are crucial for achieving lasting success in Xanax recovery.
There is no single medication, but doctors often use a long-acting benzodiazepine like diazepam (Valium) to manage withdrawal during a gradual, medically supervised taper.
Alprazolam addiction is treated with a slow, medically supervised taper off the drug, combined with intensive therapy, counseling, and long-term supportive care. This approach safely manages withdrawal and addresses the psychological roots of the addiction.
A “Xanax hangover,” which can include drowsiness and brain fog, is a sign of the drug’s lingering effects. The only way to resolve this is to stop misusing the medication under medical guidance. Proper hydration, rest, and a supervised taper can help reduce these effects.
In a hospital setting, Flumazenil may be used in emergencies to reverse the sedative effects of a benzodiazepine overdose. However, it is not used for the long-term treatment of addiction.
At District Behavioral Health Group, we provide evidence-based care for individuals struggling with xanax addiction and co-occurring mental health challenges. Our nationwide recovery network ensures a clear, connected treatment path, offering support at every stage of recovery. From detox to long-term outpatient care, our programs are designed to restore health, stability, and independence.
Our comprehensive programming includes:
Medication-Assisted Detox: Safe, medically supervised detox to manage xanax withdrawal symptoms.
Crisis Intervention & Stabilization: Immediate care to ensure safety during moments of crisis.
Inpatient & Residential Programs: 24/7 structured treatment with therapy, medical support, and daily routines in a healing environment.
Partial Hospitalization Programs (PHP): Intensive daytime therapy without overnight stays.
Intensive Outpatient Programs (IOP): Flexible part-time treatment balancing therapy with daily life.
Outpatient Programs (OP): Continued therapy to maintain recovery while living independently.
If you or someone you love is struggling with xanax addiction, call our caring team today at (888) 707-6073 and begin the path toward recovery.
Sources
[1] https://www.ncbi.nlm.nih.gov/books/NBK538165/
[2] https://americanaddictioncenters.org/xanax-treatment
[3] https://www.drugs.com/pro/xanax.html
[4]https://www.hopkinsmedicine.org/health/conditions-and-diseases/anxiety-disorders/xanax-addiction
[5] https://clincalc.com/drugstats/Drugs/Alprazolam
[5] https://www.cdc.gov/drugoverdose/data/prescribing.html
[6] https://www.addictionhelp.com/benzodiazepines/xanax/statistics/
[7] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6354096/
[8] https://alignsonoma.com/xanax-addiction-statistics/
[9] https://grovetreatment.com/addiction/drug/xanax/
[10] https://alpaswellnesscenters.org/xanax-addiction/
[11] https://www.samhsa.gov/data/sites/default/files/reports/rpt47095/National%2520Report/National%2520Report/2023-nsduh-annual-national.htm
[12] https://www.gatewayfoundation.org/what-we-treat/drug-abuse-treatment/xanax-addiction/
Check out our addiction recovery blog to learn more about substance use disorders and how to get effective treatment.

We strive to provide a comfortable, home-like environment during your recovery journey. Browse our facility images below to take a look at our upscale residential facilities.
Paying Out Of Pocket without Insurance
If you can’t pay your co-pay amount
Paying Out Of Pocket with Insurance
(Depending on insurance plan)
View our wide selection of accepted providers. Don’t see yours? Call our admissions team for help.











Whether you’re seeking help for yourself or a loved one, our admissions team is available 24/7 to answer your questions and guide you toward the right care.

| March | 2026 | |||||
|---|---|---|---|---|---|---|
| March 2026 | ||||||
| SSunday | MMonday | TTuesday | WWednesday | TThursday | FFriday | SSaturday |